Infant and Early Childhood Mental Health and Early Intervention (Part C): Policies and practices for supporting the social and emotional development and mental health of infants and toddlers in the context of parent-child relationships
Updated November 18, 2025, 12:15 PMAbstract

This briefing paper explores Infant and Early Childhood Mental Health (IECMH) policies and practices that state early intervention (Part C) programs may consider implementing to meet the social-emotional and mental health needs of infants and toddlers in the context of relationships with their parents and other caregivers.
Suggested Citation
Early Childhood Technical Assistance Center (2022). Infant and early childhood mental health and early intervention (Part C): policies and practices for supporting the social and emotional development and mental health of infants and toddlers in the context of parent-child relationships. FPG Child Development Institute, University of North Carolina. https://ectacenter.org/topics/iecmh/iecmh-partc.asp
The ECTA Center is a program of the FPG Child Development Institute of the University of North Carolina at Chapel Hill, funded through cooperative agreement number H326P220002 from the Office of Special Education Programs, U.S. Department of Education. Opinions expressed herein do not necessarily represent the Department of Education's position or policy. Project Officer: Julia Martin Eile
Contributors
This briefing paper was jointly developed and endorsed by the following organizations:
Acknowledgements
Early Childhood Technical Assistance Center (ECTA)
Andy Gomm, Christina Kasprzak, Evelyn Shaw, Alex Lazara, Sonia Sabater
The Alliance for the Advancement of Infant Mental Health (AAIMH)
Joy Browne, Nichole Paradis
The IDEA Infant & Toddler Coordinators Association (ITCA)
Maureen Greer, Sharon Loza
Georgetown University Center For Children and Families (CCF)
Elisabeth Wright Burak
Georgetown University Center for Child and Human Development (CCHD)
Neal Horen, Toby Long, Lauren Rabinovitz
National Center for Pyramid Model Innovations (NCPMI)
Lise Fox, Amy Hunter
National Center for Children in Poverty (NCCP)
Daniel Ferguson, Sheila Smith
University of Massachusetts
Kirsten Sippel-Klug (Fellow)
ZERO TO THREE
Therese Ahlers, Debbie Cheatham, Julie Cohen, Meghan Schmelzer, Lindsay Usry
Executive Summary

The COVID-19 pandemic brought growing attention to the importance of the social-emotional and mental health needs of children, parents, and caregivers.
There is also a growing recognition of the importance of healthy social-emotional development and the behavioral and mental health of young children, as well as the critical nature of early relationships with parents and other caregivers. At the same time, there has been a growing understanding of the impact of adverse childhood experiences, including trauma and toxic stress, that can affect brain development and have lifelong impacts if not addressed.
Addressing the social and emotional development of infants and toddlers with and at-risk for developmental delays and disabilities is a requirement of the Individuals with Disabilities Education Act (IDEA).
In this paper, we examine an array of infant and early childhood mental health (IECMH) policies and practices that state early intervention (Part C) programs may consider implementing to effectively support the social-emotional development and mental health needs of eligible children, that recognizes the importance of nurturing early relationships as key to the child's social-emotional wellbeing.
While this briefing paper is targeted at state early intervention (Part C) programs and addresses opportunities to be implemented at the state level—we believe that regional and local early intervention agencies can implement some of these policies and practices at the local level. We also know that collaborative partnerships will be needed for state early intervention (Part C) programs to move IECMH policies and practices forward. Key partners include state children's mental health and/or IECMH leaders, associations of infant mental health, funders (for example, Medicaid, philanthropic organizations), parent organizations, advocates, and other early learning and care programs.

This briefing paper includes a focus on information, resources, and potential opportunities that early intervention (Part C) can use to enhance services to infants and toddlers and their families across the following sections:
Introduction
This section establishes foundation information about early experiences, social-emotional development and mental health of young children, including the Importance of early relationships, the growing understanding of the impact of adverse childhood experiences and toxic stress, as well as strategies to mitigate those effects through trauma-informed care and services and practices that promote the resilience of young children through supporting strong nurturing relationships with adults. We provide a look at developmental delay, disability, and parenting, and the need to recognize and address perinatal mood disorders like postpartum depression.
An overview of early intervention Part C and IECMH provides foundational information on the key principles and practices of early intervention (Part C) and IECMH, as well as a look at the intersection between early intervention Part C and IECMH.
Referral, Screening, Assessment, and Eligibility
This section explores opportunities to include social-emotional development screening tools and expand child find and outreach efforts to promote referrals of children at-risk for social-emotional issues resulting from abuse and/or neglect and other early childhood trauma.
We also examine effective assessment tools for addressing social-emotional development and address when teams should include a mental health professional, or someone trained in IECMH as part of the assessment team. We also examine eligibility criteria for early intervention (Part C) and the potential of expanding diagnosed/established conditions lists to include additional IECMH conditions that have a high likelihood of leading to developmental delays and how diagnostic classification systems DC:0–5 can be used to identify such conditions. Another eligibility topic explored is the option for states to include an at-risk category that can include family and environmental risk factors that may lead social-emotional delays.
Services and Practices
This section includes services and practices that fall into the framework of:
- IECMH promotion;
- IECMH preventive-intervention; and
- IECMH treatment and provides an overview of an array of evidence-based models and approaches that can be provided directly by early intervention (Part C) or through partnerships with other organizations.
Workforce Development
This section addresses professional development that ranges from universal training for all early intervention practitioners, supervisors, and administrators on foundational IECMH topics, to training on evidence-based services and practices for some EI practitioners, including mental health professionals. We also address how state early intervention (Part C) programs may embed IECMH competencies into existing state early intervention competencies and how states may encourage and support Infant Mental Health (IMH) endorsement. Promoting regular and ongoing reflective supervision/consultation (RS/C) is explored to support practitioners working through the feelings and emotions that they experience from working closely with infants and toddlers and their families and that also leads to growth in their practice.
Funding, Partnership, and Collaboration
This section examines funding opportunities to provide evidence-based services, supports (for example, RS/C), and infrastructure (for example, public awareness, professional development). This includes state funding, Medicaid, private insurance, philanthropic funding, and cost-sharing braiding of funding through partnerships with other programs and organizations.
Implementation Strategies
This section provides state early intervention (Part C) programs with strategies they can use to implement the IECMH policies and practice opportunities addressed in this policy brief, with an emphasis on working in collaboration with other programs and agencies.
Appendix A: State Spotlights
This section highlights examples of state early intervention (Part C) programs that have taken steps to promote IECMH policies and practices to support the social-emotional development and mental health needs of infants and toddlers and support parent-child relationships. This represents just a few of the states that could have been spotlighted but hope these state-specific examples provide ideas for how states can move this work forward.
Appendix B: State Early Intervention (Part C) and IECMH Planning Tool
This tool assists state teams in examining the status of IECMH policies and practices, as well as which activities they want to prioritize and together explore possible next steps. This tool synthesizes all IECMH opportunities addressed throughout this paper.
By incorporating IECMH policies and practices within early intervention (Part C) and partnering with other programs and organizations to meet the social-emotional and mental health needs of infants and toddlers through providing evidence-based IECMH services to families, we can address challenges and recommendations presented by the U.S. Department of Education:
"Early childhood programs that actively involve families, serve children in natural contexts where possible, incorporate evidence-based interventions, and take a comprehensive approach to treatment are associated with greater improvements in mental health outcomes."
"There is a unique opportunity to reconceptualize the role of schools and programs in creating nurturing environments for children, students, families, and educators to address the mental health needs and overall wellbeing of children and students."
These challenges and recommendations are summarized in Figure 1.
Figure 1. Challenges and Recommendations for the Provision of Mental Health Services for Early Childhood and School Age Children
| Challenges | Recommendations |
|---|---|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Glossary
- Adverse Childhood Experiences (ACEs)
- Potentially traumatic events, including abuse and neglect, as well as other family challenges that have been shown to lead to negative developmental, health and mental health outcomes.
- Caregiver
- Other adults who care for the child in addition to the parents including extended family members, child care, Early Head Start and other early care and education professionals including family home child care providers, nannies, and babysitters.
- Clinician
- Licensed mental health professionals including counselors, therapists, clinical social workers, and psychologists who can assess and diagnose mental health conditions and provide therapeutic intervention or treatment.
- Early Intervention
- Services provided in accordance with the Individuals with Disabilities Education Act (IDEA) Part C for children birth to age 3 with and at-risk for developmental delays and disabilities and their families.
- Endorsement
- A credential that recognizes practitioners' knowledge base, experiences, and demonstration of competency. It does not replace licensure or certification, but instead is meant as evidence of specialization in a particular field.
- Infant and Early Childhood Mental Health (IECMH)
- The developing capacity of the child ages birth–5 years to form close and secure adult and peer relationships; experience, manage, and express a full range of emotions; and explore the environment and learn—all in the context of family and community.
- IECMH Consultation
- A support service provided to individuals and teams to address the social-emotional needs and mental health concerns of infants, young children and their families within various programs and settings.
- Individual Family Service Plan (IFSP)
- A written plan developed with the family in accordance with the requirements of Part C of IDEA. An IFSP includes the early intervention services to be provided along with the outcomes and strategies to support eligible infants and toddlers and their families.
- Infant Mental Health (IMH)
- An interdisciplinary approach to supporting the social and emotional development and mental health needs of infants and toddlers (birth to age 3) in the context of nurturing relationships with parents and other caregivers. The broader term Infant and Early Childhood Mental Health (IECMH) is used in this paper.
- Family
- Any type of family, including, but not limited to: single parents, separated and divorced parents, co-parents, legal guardians, multigenerational, foster families, and adoptive families.
- Parent
-
IDEA Regulations 34 CFR §303.27 defines a parent as:
- a biological or adoptive parent of a child;
- a foster parent;
- a guardian generally authorized to act as the child's parent, or authorized to make early intervention, educational, health or developmental decisions for the child (but not the State if the child is a ward of the State);
- an individual acting in the place of a biological or adoptive parent (including a grandparent, stepparent, or other relative) with whom the child lives, or an individual who is legally responsible for the child's welfare; or
- a surrogate parent who has been appointed.
- Reflective Supervision/Consultation (RS/C)
- Regular, ongoing sessions where an individual or group of practitioners meet with a professional who is trained in RS/C, and given the opportunity to reflect on emotions and thoughts regarding their work. As well as providing support when challenging and painful feelings arise. The goal of RS/C is to integrate learning, and improve quality of practice. This support may be provided by a consultant outside of the agency.
- Social-Emotional and Mental Health Needs
- The broad array of needs that support healthy social and emotional development and address the needs of young children who have experienced adverse childhood experiences and other trauma that may lead to developmental concerns.
- Social-Emotional Development
- The child's ability to:
- identify and understand their own feelings;
- accurately read and comprehend emotional states in others;
- manage strong emotions and their expression in a constructive manner;
- regulate their own behavior;
- develop empathy for others; and
- establish and maintain relationships.
- State Early Intervention (Part C) Program
- The designated lead agency for the administration of the statewide system of services and supports provided to eligible infants and toddlers with or at-risk for developmental delay or disabilities and their families in accordance with Part C of IDEA.
- Toxic Stress
- Negative effects on development, behavior, and health across the lifespan caused by experiencing strong, frequent and prolonged exposure to adverse childhood experiences, and other trauma that occur in the absence of nurturing support from an adult caregiver as a young child or infant. Toxic stress can be diminished when the infant/child experiences a nurturing adult relationship to buffer those toxic events.
- Trauma
- A body or life-threatening event experienced by a young child that can cause a psychological response. Such events may include abuse and neglect, domestic violence, as well as accidents, natural disasters, or medical events. Young children may not be able to express their response to trauma verbally due to their age.
Introduction

This section provides background and foundational information regarding:
- the science of social and emotional development and mental health of young children;
- an overview of early intervention (Part C) and infant and early childhood mental health (IECMH); and
- the intersection between early intervention (Part C) and IECMH.
Early Experiences, Social-Emotional Development and Mental Health of Young Children
The Importance of Early Relationships
There is consensus in the scientific community regarding the key role that early childhood experiences play in determining the foundational organization and capabilities of the brain.
According to the Center on the Developing Child at Harvard University:
"Early experiences affect the nature and quality of the brain's developing architecture by determining which circuits are reinforced and which are pruned through lack of use."
Neuroscience and developmental science research have determined that children develop within relationships that begin with the family but also involve other adult caregivers, including extended family members and early care and education professionals. Early relationships have an important influence on a child's brain structure and function that affect virtually all aspects of their development. The National Scientific Council on the Developing Child describes development as occurring within an "environment of relationships" that "provides a foundation of capacities that children will use for a lifetime".
The Council further concluded:
"Healthy development depends on the quality and reliability of a young child's relationships with the important people in his or her life, both within and outside the family. Even the development of a child's brain architecture depends on the establishment of these relationships.
Growth-promoting relationships are based on the child's continuous give-and-take ("serve and return" interaction) with a human partner who provides what nothing else in the world can offer—experiences that are individualized to the child's unique personality style; that build on his or her own interests, capabilities, and initiative; that shape the child's self-awareness; and that stimulate the growth of his or her heart and mind."
A 2020 strategic brief published by the FrameWorks Institute, in collaboration with David Willis, MD and colleagues at the Center for the Study of Social Policy explore the emerging use of the term early relational health to galvanize the interest of health and early childhood providers around the importance early relational experiences:
"In fact, early relational health builds upon decades of research from the fields of child development, infant mental health and neurodevelopment that has established the centrality of relationships between caregivers and very young children for future health, development and social-emotional wellbeing."
"Stable, caring relationships are essential for healthy development. Children develop in an environment of relationships that begin in the home and include extended family members, early care and education providers, and members of the community. Studies show that toddlers who have secure, trusting relationships with parents or non-parent caregivers experience minimal stress hormone activation when frightened by a strange event, and those who have insecure relationships experience a significant activation of the stress response system. Numerous scientific studies support these conclusions: providing supportive, responsive relationships as early in life as possible can prevent or reverse the damaging effects of toxic stress."
Adverse Childhood Experiences and Toxic Stress
During the early childhood period, the brain is exquisitely sensitive to the positive aspects of caregiving, but this also renders it vulnerable to stressors.
Infants exposed to early life stressors, including domestic violence, caregiver substance use disorders, severe relational challenges, caregiver abuse, neglect, and lack of caregiver attunement can lead to developmental and health problems (Hambrick et al., 2019).
Adverse Childhood Experiences (ACEs) are traumatic events experienced by children that have been shown to lead to a range of poor health, and educational and mental health outcomes later in life. ACEs include abuse (physical, emotional, sexual), neglect (physical or emotional) and household challenges (incarceration, mental illness, substance use disorder or dependence, absence due to separation or divorce, and intimate partner violence).
Dr. Nadine Burke Harris, Surgeon General of California, in her testimony to Congress (2019), said:
"A robust body of literature demonstrates that ACEs are highly prevalent, strongly associated with poor childhood and adult health, mental health, behavioral and social outcomes and demonstrate a pattern of high rates of intergenerational transmission…
…the higher the ACE score, the more likely the individual is to struggle with mental health issues such as depression, post-traumatic stress disorder, anxiety, sleep and eating disorders, and to engage in risky behaviors such as early and high-risk sexual behavior and substance abuse."
ACEs and other early traumatic experiences are associated with toxic stress. While mild-to-moderate short-lived stress and the ability to cope with adversity are an important part of healthy early childhood development, ongoing and high levels of stress, without protective adult support, can lead to long-lasting negative developmental consequences. Science has shown that the neural connections in areas of the brain for learning and reasoning are weaker and fewer in the presence of prolonged activation of stress hormones.
Trauma-Informed Care
A trauma-informed care approach is characterized by an understanding that behaviors that result from trauma for the child or parent are responded to with "what happened to you?", not "what's wrong with you?" and a recognition that these individuals may need intervention/treatment.
SAMHSA provides important assumptions to guide professionals and programs in implementing a trauma-informed approach:
"A program, organization, or system that is trauma-informed realizes the widespread impact of trauma and understands potential paths for recovery; recognizes the signs and symptoms of trauma in clients, families, staff, and others involved with the system; and responds by fully integrating knowledge about trauma into policies, procedures, and practices, and seeks to actively resist re-traumatization."
The National Center for Pyramid Model Innovations (NCPMI) addresses how the pyramid model can be used to support children who are impacted by trauma and includes a checklist that provides guidance on practices related to:
- nurturing and responsive relationships;
- creating safe learning environments;
- creating calm, predictable transitions;
- helping children regulate their emotions and express their feelings appropriately; and
- providing intensive interventions that consider the child's experiences
Resilience
Positive health and developmental outcomes have been shown to be influenced by the child having at least one stable and committed relationship with a supportive parent, caregiver, or other adult. Stable, committed, and responsive relationships have been shown to help a child who has experienced negative experiences and/or toxic stress build resilience.
The Center on the Developing Child at Harvard University stresses the importance of at least one stable and committed relationship between the child and a supportive parent, caregiver, or other adults:
"The single most common factor for children who develop resilience is at least one stable and committed relationship with a supportive parent, caregiver, or other adult. These relationships provide the personalized responsiveness, scaffolding, and protection that buffer children from developmental disruption. They also build key capacities—such as the ability to plan, monitor, and regulate behavior—that enable children to respond adaptively to adversity and thrive. This combination of supportive relationships, adaptive skill-building, and positive experiences is the foundation of resilience."
In their exploration of childhood trauma, psychiatrist Dr. Bruce Perry and Maia Szalavitz conclude that:
"…the more healthy relationships a child has, the more likely he will be to recover from trauma and thrive."
Developmental Delay, Disability, and Parenting

Families who have a young child with a developmental delay or disability may experience a variety of stressors. These stressors may include social isolation, social stigma, feelings of guilt, worry about the ability of their child to make friends, worry about the ability of their child to live an independent life, and a loss of parental career and social opportunities. It is important for early intervention practitioners to be sensitive to these stressors and the emotional experience of parents, while understanding that this will differ across families.
Certain diagnoses, such as autism spectrum disorder (ASD), can cause parental stress and may challenge parent-child attachment. A meta-analysis of the impact of parenting stress found a significant difference between the stress of parents of children with ASD, as well as children diagnosed with other disabilities, compared to parents of typically developing children (Hayes & Watson, 2013).
Additionally, parents with a child in the Newborn/Neonatal Intensive Care Unit (NICU) may themselves experience post-traumatic stress (Schecter et al., 2019) that may affect the parent-child relationship (Beck, 2015), and they often experience postpartum depression.
Professionals can support parents of young children with a developmental delay or disability by listening to their story and following the family's lead on the use of words to describe how they see their child's and family's situation. Some parents may benefit from counseling.
"Counseling ought to empower parents using the dialogue that they articulate rather than reflecting the practitioners' assumptions about what they imagine it to be like, based on the tragic concept of disabilities."
Early intervention teams must be sensitive to the potential stress and challenges experienced by parents of children with developmental delays or disabilities, as well as their need for support. Families can benefit from connecting with other families who have had similar experiences through a referral to a Parent Training and Information Center. Some families with significant stress or emotional challenges may also benefit from family counseling.
Overview of Early Intervention Part C and IECMH
Early Intervention (Part C) Foundations
Early intervention, in accordance with the Individuals with Disabilities Education Act (IDEA) Part C, provides services for infants and toddlers, from birth to age three with and at-risk for developmental delays and disabilities, and their families. Each year, state early intervention programs ensure access to, and participation in, the statewide Part C system (34 CFR §303.212).
State early intervention (Part C) programs are located within different state lead agencies, including education, health, social services, developmental disabilities and increasingly within early childhood agencies, along with other early learning and care programs for children birth to age 5 and their families that consolidates or creates a new agency to promote early childhood governance as outlined in the Build Initiative's A Framework for Choosing a State-Level Early Childhood Governance System.
A System Framework for Building High-Quality Early Intervention and Preschool Special Education Programs supports states to address "What does a state need to put into place to encourage/support/require local implementation of evidence-based practices that result in positive outcomes for young children with disabilities and their families?". The framework includes quality indicators within six system components (see Figure 2).
Figure 2. Early Intervention (Part C) System Framework
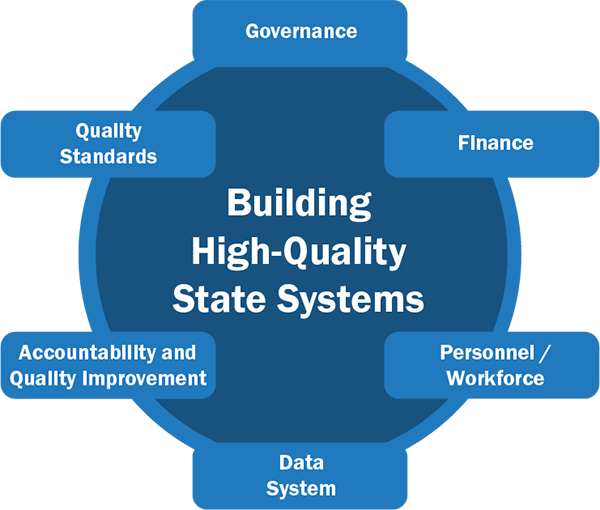
The federal IDEA Part C statute and IDEA Regulations establish the requirements for the provision of early intervention and the rights of families under the IDEA Part C. State early intervention (Part C) programs develop State Part C Regulations and Policies, procedures and guidance that includes state's eligibility criteria, evaluation and assessment requirements, and personnel qualifications.
This briefing paper addresses how states may examine their policies and procedures in these areas to effectively address the social-emotional, developmental, and mental health needs of eligible infants and toddlers and provide evidence-based services to support parent-child relationships.
Early intervention services support parents and other caregivers to promote the child's development within daily activities and routines (natural environments). Increasingly early intervention practitioners use a coaching approach. How states provide early intervention is addressed in the Seven Key Principles and Practices for Providing Early Intervention Services in Natural Environments that were developed by a national workgroup (see Figure 3). State early intervention (Part C) programs may also provide training and support for the implementation of several research-based service delivery approaches or models.
Figure 3. Early Intervention Key Principles and Practices
- Infants and toddlers learn best through everyday experiences and interactions with familiar people in familiar contexts.
- All families, with the necessary supports and resources, can enhance their children's learning and development.
- The primary role of a service provider in early intervention is to work with and support family members and caregivers in children's lives.
- The early intervention process, from initial contacts through transition, must be dynamic and individualized to reflect the child's and family members' preferences and learning styles.
- IFSP outcomes must be functional and based on children's and families' needs and family-identified priorities.
- The family's priorities, needs and interests are addressed most appropriately by a primary provider who represents and receives team and community support.
- Interventions with young children and family members must be based on explicit principles, validated practices, best available research, and relevant laws and regulations.
IECMH Foundations
It can be helpful to look at definitions of IECMH that both focus on the early social and emotional development of infants, toddlers, and young children in the context of relationships, as well as the emerging multidisciplinary professional field of Infant Mental Health.
ZERO TO THREE defines IECMH as:
"…the capacity of a child from birth to age five to
- experience, express and regulate emotions;
- form close, secure interpersonal relationships; and
- explore his/her environment and learn, within the context of family and cultural expectations."
The Michigan Association for Infant Mental Health gave this definition for IECMH:
"…an interdisciplinary field dedicated to understanding and promoting the social and emotional well-being of all infants, young children, and families within the context of secure and nurturing relationships. Infant mental health also refers to the social and emotional well-being of an infant or toddler within the context of a relationship, culture, and community."
The Handbook of Infant Mental Health provides another definition:
"…infant mental health may be defined as a multidisciplinary professional field of inquiry, practice, and policy concerned with alleviating suffering and enhancing the social and emotional competence of young children. Infant mental health is multidisciplinary because the complex, interrelated nature of human development and its deviations requires expertise and conceptualizations beyond the capabilities of any particular discipline."
The infant mental health approach originated in the 1960s with children with disabilities and their families.
The work of Selma Fraiberg and colleagues with parents of young children who were blind and visually impaired concluded that early experience is crucial to development and that there is a need to focus on infants and parents together to enhance the baby's development (Weatherston & Shirilla, 2002).
IECMH supports and services can be conceptualized as a continuum or framework that includes:
- promotion of healthy social and emotional development for all young children;
- preventive-intervention services through social and emotional developmental screening, parenting support, home visiting and intervention, to address family risk factors (for example, abuse and neglect, substance use disorder, domestic violence, parental mental health issues), early identification of concerns; and
- treatment using evidence-based dyadic clinical treatment to address the parent-child relationship when their interactions are determined to have a negative effect on the mental health of the young child.
The Handbook of Infant Mental Health (Zeanah, 2019) includes guiding principles for Infant Mental Health (IMH), which are presented in Figure 4.
Figure 4. IMH Guiding Principles
- Infant mental health is concerned with healthy social-emotional development.
- Relationships form the fundamental building blocks of social and emotional development: early experiences matter.
- Infant-caregiver relationships provide the framework for assessment and intervention in infant mental health.
- Infant mental health aims to identify, establish, and sustain positive developmental capacities.
- Assessment and intervention are strength-based: Strengths are used to minimize risk and support parent, infant and family competency.
- Intervention always includes prevention: Intervention aims to reduce distress and maladaptive behaviors in the present and restore positive developmental trajectories and build competence and resilience for future functioning.
- Cultural beliefs define assumptions about important aspects of childrearing.
- Families must be involved in the planning and delivery of services.
- Personal, professional, and program values permeate all aspects of infant mental health.
- A comprehensive continuum of services is needed, and cross-system collaboration is essential: to be effective, policies and programs must reflect and respond to the relational needs of infants.
Case Studies in Infant Mental Health: Risk, Resiliency, and Relationships (Weatherston & Shirilla, 2002) defines IMH skills and strategies that are rooted in a psychodynamic and clinical approach that help differentiate the role of IMH practice from other work with young children and their families. They include:
- wondering about the parent's thoughts and feelings related to the presence and care of the infant and the changing responsibilities of parenthood;
- wondering about the infant's experiences and feelings in interaction with and relationship to the caregiving parent;
- listening for the past as is expressed in the present-inquiring and talking;
- allowing core relational conflicts and emotions to be expressed by the parent-holding, containing, and talking about them as the parent is able;
- attending and responding to parental histories of abandonment, separation, and unresolved loss as they affect the care of the infant, the infant's development, the parent's emotional health, and the early developing relationship;
- attending and responding to the infant's history of early care within the developing parent-infant relationship; and
- identifying, treating, and/or collaborating with others, if needed, in the treatment of disorders of infancy, delays and disabilities, parental mental illness, and family dysfunction.
Professionals with a variety of qualifications and from various disciplines may play the role of an infant mental health practitioner. The Workforce Development section of this paper explores interdisciplinary professional development and an endorsement process available in some states to promote IMH competencies.
Intersection Between Early Intervention Part C and IECMH
Multidisciplinary early intervention (Part C) teams support and coach parents and other caregivers to promote a child's development within daily routines, activities, and places. IECMH practitioners utilize promotion, prevention, and treatment strategies to address the child's mental health and focus on the parent-child dyadic relationship.
Both early intervention (Part C) and IECMH systems can be seen as addressing the social-emotional development of infants and toddlers and as promoting the parent-child relationship. Figure 5 shows this intersection, which may be larger than illustrated.
Figure 5. Intersection between Early Intervention Part C and IECMH
- EI Part C
- Support and coach parents to promote their child's development within daily routines
- Multidisciplinary team approach
- IECMH
- Promotion, prevention, treatment of mental health
- Focus on the parent-child dyadic relationship
- Both
- Social and emotional development
- Parent-child relationship
Knowing that the social-emotional and mental health needs of infants and toddlers are supported through nurturing parent-child relationships, early intervention should use strategies that bolster the parent-child relationship and social-emotional capacities of the infant-toddler, which will promote growth in all areas of development.
Several state early intervention (Part C) programs have begun to promote IECMH policies and make available evidence-based IECMH services—either by early intervention teams or through collaboration and partnerships with other mental health organizations. We have spotlighted several states throughout this paper.
Referral, Screening, Assessment, and Eligibility

This section addresses ways to support the social-emotional development and mental health needs of infants and toddlers by early intervention (Part C) programs through:
- expanded referrals of children with social and emotional delays and the Child Abuse Prevention and Treatment Act (CAPTA) requirements;
- screening for social and emotional developmental delays, family risk factors and postpartum or perinatal mood disorders;
- effective evaluation and assessment of social-emotional development and the parent-child relationship—including use of appropriate tools and including team members with mental health expertise; and
- eligibility criteria, including use of the at-risk category, the inclusion of mental health established conditions, and use of diagnostic classification for IECMH conditions.
Referral and Screening
Referrals of Children with Social and Emotional Delays

While state early intervention (Part C) programs are required under IDEA Regulations 34 CFR §303.302 and 34 CFR §303.303 to establish a comprehensive statewide child find system to identify, locate, and evaluate all infants and toddlers who may be eligible for services.
Based on the state's definition of developmental delay or disability, states may consider expanding strategies to specifically focus on identifying infants and toddlers with social-emotional delays.
Supporting Social-Emotional and Mental Health Needs of Young Children Through Part C Early Intervention: Results of a 50-state Survey found that 30 state early intervention (Part C) programs provide online and in-person training to referral sources that includes information about referring children with social-emotional concerns (Smith et al., 2020).
Early intervention practitioners may not have received specific training in social-emotional development or infant and early childhood mental health and therefore may not feel they are able to discuss the importance of referring young children where there is a concern in this area of development.
The referral of infants and toddlers with social-emotional concerns can be increased if state early intervention focus child find and outreach efforts to social service providers that address homelessness, domestic violence, teen parenting, substance abuse disorder, and adult mental health. As delays in social-emotional development may not be as obvious as those in other domains, state early intervention (Part C) programs can help health, early child and social service providers to be aware of social-emotional "red flags" and incorporate developmental screening that includes social-emotional development.
Outreach to birth hospitals, including newborn and pediatric intensive care units, can help identify parents who have experienced trauma related to their baby's premature birth, birth trauma, or other medical/birth complications.
For more information, see Michigan in Appendix A: State Spotlights.
Referrals Related to the Child Abuse, Prevention and Treatment Act (CAPTA)
Reauthorization of both CAPTA in 2003, and IDEA in 2004 and subsequent IDEA Regulations 34 CFR §303.303 require states to establish procedures for the referral of children to early intervention (Part C) for screening or evaluation when abuse and neglect is substantiated by the child welfare agency.
The public policy effort to systematically refer young children who have experienced abuse and neglect or who were affected by substance use in utero can be seen as stemming from the publication of the seminal 2000 book From Neurons to Neighborhoods: the Science of Early Childhood Development, in which the authors state:
"Decades of research on the early development of the brain convey a powerful and sobering message about its susceptibility to harmful influences. This leads us to be deeply concerned about the well-being of young children who suffer from extreme deprivation, inadequate nutrition, neurotoxic exposures, or other insults that can cause significant (although sometimes subtle) brain damage during the prenatal or early childhood years…
…and early intervention efforts should be substantially expanded to reduce documented risks that arise from harmful prenatal and early postnatal neurotoxic exposures, as well as from seriously disrupted early relationships due to chronic mental health problems, substance abuse, and violence in families."
Subsequent research has shown that around 40% of young children in child welfare have a developmental or behavioral problem that would likely qualify them for early intervention services. However, only 13% of infants and toddlers received developmental or behavioral intervention (Stahmer et al., 2005).
IDEA Regulations 34 CFR §303.303 were amended to additionally require state early intervention (Part C) programs to develop policies and procedures for the referral of young children who are "Identified as affected by illegal substance abuse, or withdrawal symptoms resulting from prenatal drug exposure".
In Child Maltreatment 2019, the U.S. Department of Health & Human Services, Administration for Children and Families reported that 28 states and territories reported on the number of eligible children referred to early intervention (Part C) from child welfare and several of those cited low percentages in 2019 (U.S. Department of Health & Human Services, Administration for Children and Families, Administration on Children, Youth and Families, Children's Bureau, 2021, p.81).
Five years after the passage of the amendments, a 2016 study showed that fewer than a fifth of all children with a substantiated case of abuse or neglect (18.2%) received a referral to early intervention Part C (Johnson-Motoyama et al., 2016) showing that there is much work to be done to ensure that all children are referred.
State early intervention (Part C) programs worked in collaboration with state child protection/child welfare agencies in the mid-2000s to develop CAPTA referral policies and procedures. These policies and procedures should be revisited to ensure they are effective and being followed. Data analysis and field interviews with early intervention and child welfare staff can be used to guide needed revisions to policies, procedures, and training to support timely and effective referrals, including effective screening and evaluations.
The Comprehensive Addiction and Recovery Act (CARA) of 2016 included changes to CAPTA, which require states to develop a Plan of Safe Care (POSC) for infants identified as affected by parental substance use disorder, showing withdrawal symptoms, or Fetal Alcohol Spectrum Disorders (FASD). The POSC is to ensure the safety and well-being of such infants following discharge from the hospital and addresses the health and treatment needs of the infants and affected family members or caregivers, as well as referral to early intervention Part C services and/or other early childhood services.
For more information, see Rhode Island in Appendix A: State Spotlights.
Screening for Social and Emotional Development

Early intervention (Part C) programs may include developmental screening to identify developmental concerns in young children as part of their child find efforts, however they also promote collaboration with statewide community level efforts to offer developmental screening.
These wider developmental screening efforts include primary health care providers and early learning and care providers (for example, home visitors, child care providers, Early Head Start) in helping to identify developmental concerns in infants and toddlers and making timely referrals to early intervention programs.
Research has shown that screening tools focused on social-emotional development are more effective than broad developmental screening tools for identifying children who need further evaluation of social-emotional concerns (Williams et al., 2017). Some referral sources (health, child care, Early Head Start, home visiting, etc.) increasingly use screening tools for social-emotional development, such as the Ages & Stages Questionnaires: Social-Emotional, Second Edition (ASQ:SE-2), which is likely to increase the number of referrals of children with possible social and emotional developmental challenges. A national survey conducted by the National Center for Children in Poverty in 2020 found that eight state early intervention (Part C) programs require the use of the ASQ:SE-2 and another 30 states recommend its use (Smith et al., 2020).
Procedures around screening differ from state-to-state when it comes to CAPTA referrals, with either child welfare or early intervention personnel conducting the screening, while other states conduct a full multidisciplinary developmental evaluation without requiring a screening. Only nine states "require the use of a social-emotional screening and/or evaluation tool for children involved in a substantiated case of abuse or neglect, although nearly half recommend a social-emotional tool" (Smith et al., 2020, p.7).
In Meeting the Social-Emotional Needs of Infants and Toddlers: Guidance for Early Intervention Program Providers and Other Early Childhood Professionals, the Clinical Clues of Social-Emotional Development Delays and Disabilities Chart include items and behaviors that were cross-referenced from a variety of social-emotional screening and assessment tools. These clinical triggers can alert non-mental health and mental health professionals alike that "the presence of these indicators strongly suggest that a social-emotional/mental health assessment may be indicated". The list of behaviors and items are clustered into concerns about sleep, eating, comfort, relating to people, mood, emotions and feelings, self-harm, behavior, possible exposure to excessive/toxic stress, and regression (New York State Department of Health Early Intervention Program, 2017, pp.31-33).
Figure 6 includes several tools for screening for social and emotional development.
For more information, see New York in Appendix A: State Spotlights.
Figure 6. Screening Tools for Social-Emotional Development
| Tool | Age Range |
|---|---|
| Ages & Stages Questionnaire: Social-Emotional (ASQ:SE-2) | 1–72 months |
| Greenspan Social-Emotional Growth Chart | 0–42 months |
| Brief Infant and Toddler Social and Emotional Assessment (BITSEA) | 12–36 months |
Postpartum Depression Screening

Perinatal or postpartum mood and anxiety disorder (PMAD) is associated with less responsive parenting and disruption of infant-parent-child interaction; however, it often goes unaddressed (Earls, 2010). Early intervention programs can play a role in either screening or referring a parent for screening for postpartum depression. Five state early intervention (Part C) programs screen for postpartum depression and 18 states reported that they refer mothers for evaluations or treatment of maternal depression to other health or mental health providers (Smith et al., 2020).
Early intervention teams should be aware of postpartum depression risk factors, including:
- depression or anxiety during pregnancy;
- stressful life events experienced during pregnancy or in the postpartum period;
- traumatic birth experience
- preterm birth/infant admission to neonatal intensive care (NICU);
- low levels of social support;
- previous history of depression; and
- breastfeeding problems.
The Edinburgh Postnatal Depression Scale (EPDS) is commonly used as a depression screening tool for postpartum depression and includes ten items and takes less than five minutes to complete (Lancaster et al., 2010).
As maternal depression can interfere with responsive parenting and contribute to problems in the parent-child relationship parent, early intervention (Part C) teams should help parents access an appropriate mental health provider based on the results of the screening that either they or another entity conducted.
Treatment services may include psychotherapy or counseling for mild-to-moderate peripartum depression and psychiatric pharmacologic treatment in moderate-to-severe cases of postpartum depression. There is also an increasing interest in screening fathers for perinatal depression (Walsh et al., 2020).
Other Family Risk Factor Screening
As part of conducing their evaluation of the child and assessment of the child and family, programs may consider screening for a range of family risk factors (for example, substance use, domestic violence, homelessness) as part of intake, whether or not they include an at-risk eligibility category. This can be considered part of the required family-directed assessment:
- A family-directed assessment must be conducted by qualified personnel in order to identify the family's resources, priorities, and concerns and the supports and services necessary to enhance the family's capacity to meet the developmental needs of the family's infant or toddler with a disability. The family-directed assessment must —
- Be voluntary on the part of each family member participating in the assessment;
- Be based on information obtained through an assessment tool and also through an interview with those family members who elect to participate in the assessment; and
- Include the family's description of its resources, priorities, and concerns related to enhancing the child's development.
New Mexico's early intervention (Part C) program uses the Environmental Risk Assessment (ERA) Tool: Assessment of environmental risk factors in families of children birth to age three during intake to determine eligibility under the state's environmental risk category as a guide intervention. The tool includes several family risk and protective factors.
Evaluation and Assessment
Tools For Assessing Social and Emotional Development
Early intervention teams use a variety of developmental assessment tools and procedures as part of the initial evaluation to determine the child's eligibility and for ongoing assessment.
Some states mandate or recommend the use of one particular tool statewide, some allow providers to select tools from an approved list, while others allow local early intervention providers to determine the assessment tool(s) to be used.
Early intervention teams should consider whether the assessment tool used adequately addresses social-emotional development, and if not, to use a supplemental tool, if allowed under state policies and procedures. It is recommended that teams consider adding a supplemental tool to assess social-emotional development in the following circumstances:
- when the referral of the child is made under CAPTA;
- when a screening tool has already identified social and emotional concerns; or
- where there are known family-related risk factors (for example, substance use disorder, domestic violence, homelessness, abuse, or neglect).
Examples of assessment tools that can be considered as supplemental tools specific to social-emotional development are included in Figure 7.
Figure 7. Assessment Tools with a Focus on Social-Emotional Development
| Tool | Age Range |
|---|---|
| Devereux Early Childhood Assessment (DECA) | 4 weeks–18 months, and preschool children ages 2–5 |
| Infant and Toddler Social and Emotional Assessment (ITSEA) | 12–36 months |
| Social-Emotional Assessment/Evaluation Measure (SEAM) | 2–66 months |
Considerations For Including a Mental Health Professional As Part of the Evaluation Team

Adding a mental health professional (for example, social worker, family counselor, psychologist) or someone trained and/or endorsed in infant mental health to the evaluation team can enhance the team's ability to assess social and emotional development.
This should be considered:
- when the referral of the child is made under CAPTA;
- when a screening tool has already identified social and emotional concerns; or
- where there are known family-related risk factors (such as substance use disorder, domestic violence, homelessness, abuse, or neglect).
A mental health professional may be accessed from a community mental health agency if not currently part of the early intervention team.
Determining whether to include a mental health professional on the evaluation team is similar to determining whether to include other disciplines (for example, speech, motor, health) based on the referral and the presenting circumstances.
In 2020, 13 states reported that they include early intervention practitioners with training or expertise in infant-toddler mental health as part of eligibility evaluation teams and 11 states reported having written guidance regarding their participation. One state explained:
"A positive screen on the ASQ:SE-2 indicates that the evaluation team should consider including a professional with a background in infant-toddler early childhood mental health and social-emotional development."
Use of the Diagnostic Classification DC:0–5
The Diagnostic Classification of Mental Health and Developmental Disorders of Infancy and Early Childhood (DC:0–5) is commonly used to classify mental health and developmental disorders in infants and young children.
DC:0–5 includes several disorders (for example, neurodevelopmental disorders; sensory processing disorders; anxiety disorders; mood disorders; obsessive compulsive disorders and related disorders; sleep, eating, and crying disorders; trauma, stress, and depression disorders, including reactive attachment disorder; posttraumatic stress disorder; relationship disorders) that are related to IECMH and that have a high likelihood of leading to a delay in social-emotional development.
Trained mental health clinicians who work as part of an early intervention team or community mental health organizations can use DC:0–5 to:
- determine the extent and nature of the relationship disruption, psychosocial stressors, and trauma they observe to be leading to social-emotional and mental health issues for the young child;
- determine if the family could benefit from evidence-based IECMH dyadic or group treatment (either within early intervention or through a referral); and
- identify conditions that would make the child eligible under the state early intervention (Part C) diagnosed/established conditions list.
In 2020, 8 state early intervention (Part C) programs reported that they require or recommend the use of DC:0–5 (Smith et al., 2020). Some states, such as Colorado, require early intervention provider agencies to employ a DC:0–5-trained mental health clinician. DC:0–5 training targets clinicians from mental health, health, and early intervention who are responsible for assessment and diagnosis (Zeanah et al., 2017).
It is helpful for early intervention teams to have a working understanding of DC:0–5 as it is commonly used by mental health and child welfare systems that may serve infants, toddlers, and their families eligible for early intervention (Part C). DC:0–5 provides a common language to use across disciplines and programs for understanding parent-child relational disruptions and guiding potential interventions and treatments for the child and family.

For more information, see Colorado in Appendix A: State Spotlights.
Other Assessment Tools Focused on the Parent-Child Relationship
Assessment tools that focus on the parent-child relationship presented in Figure 8 can be considered by early intervention teams to be used as part of the initial evaluation or ongoing assessment to determine whether the parent-child relationship has improved over time. These tools also provide ideas regarding family outcomes and strategies to be incorporated into the IFSP.
Figure 8. Assessment Tools with a Focus on the Parent-Child Relationship
| Tool | Focus | Age Range |
|---|---|---|
| Parenting Interactions with Children: Checklist of Observations Linked to Outcomes (PICCOLO) | Observable developmentally supportive parenting behaviors in four domains (affection, responsiveness, encouragement, and teaching). | 10–47 months |
| Dyadic Parent-Child Interaction Coding System (DPICS) | Behavioral coding system that measures the quality of parent-child social interactions. | 2–7 years |
| Functional Emotional Assessment Scale (FEAS) | Observational tool for practitioners to measure the emotional function of a child when supported by a caregiver, and normative measure of a child's functional, emotional, and developmental capacities. | 7–48 months |
| Emotional Availability Scales | Evaluation of adult-child relationships related to attachment. | 0–14 years |
Of these tools, the PICCOLO was found to be an appropriate, reliable, and valid measure of parenting interactions for children with a disability, as well for children developing according to age expectations. The researchers at the Center for Persons with Disabilities at Utah State University propose that the PICCOLO lends itself to a strengths-based parenting approach and suggest that including a focus on parenting increases the effectiveness of early intervention. They conclude:
"Early intervention practitioners can use PICCOLO to better understand a parent's parenting skills and to build on those behaviors that parents are already using and value."
Eligibility Criteria
State Early Intervention (Part C) Developmental Delay Criteria and Diagnosed Conditions
Under IDEA Regulations 34 CFR §303.111, state early intervention (Part C) programs establish eligibility criteria for developmental delay, with social-emotional being one of the developmental domains that is evaluated. The level of developmental delay that makes a child eligible varies from state to state.
Figure 9 shows the number of states with broad, moderate, or restrictive eligibility categories, based on state staff self-selection (IDEA Infant & Toddler Coordinators Association, 2019).
Figure 9. State Early Intervention (Part C) Eligibility Groupings
| Category | N of States | Level of Developmental Delay Included in State Eligibility Criteria | SD Below Mean in State Eligibility Criteria |
|---|---|---|---|
| Broad | 15 |
|
|
| Moderate | 20 |
|
|
| Restrictive | 16 |
|
|
States also decide which diagnosed physical or mental conditions are included in their list of diagnosed/established conditions determined as having a high probability of resulting in a developmental delay. Some states have developed extensive lists while others use the diagnosed conditions listed in IDEA Regulations 34 CFR §303.21.
The ECTA Center maintains a database of State and Jurisdictional Eligibility Definitions for Infants and Toddlers with Disabilities Under IDEA Part C, which includes the developmental delay criteria for each state. However, because the diagnosed/established conditions for some states are extensive, the database focuses on a few key diagnosed/established conditions that state early intervention (Part C) programs have included. The database also includes links to state eligibility policies and lists.
Some state early intervention (Part C) programs (including Michigan and New Mexico) have included several mental health conditions in addition to severe attachment disorders included in IDEA Regulations 34 CFR §303.21, which have been determined to have a high likelihood of leading to a developmental delay including in social-emotional development, for example:
- adjustment disorders;
- depression of infancy and early childhood;
- maltreatment/deprivation disorder;
- disorders of affect;
- mixed disorders of emotional expressiveness;
- post-traumatic stress disorder (PTSD); and
- regulatory disorder.
State early intervention (Part C) programs may consider convening a taskforce of mental health professionals to make recommendations regarding which conditions have a high probability of resulting in a developmental delay, especially social-emotional development, and therefore should be included in their diagnosed/established conditions eligibility criteria.
At-Risk Eligibility Category
IDEA Regulations allow state early intervention (Part C) programs to include in their Part C eligibility criteria infants and toddlers who are at-risk.
"At-risk infant or toddler means an individual under three years of age who would be at-risk of experiencing a substantial developmental delay if early intervention services were not provided to the individual. At the State's discretion, at-risk infant or toddler may include an infant or toddler who is at risk of experiencing developmental delays because of biological or environmental factors that can be identified (including low birth weight, respiratory distress as a newborn, lack of oxygen, brain hemorrhage, infection, nutritional deprivation, a history of abuse or neglect, and being directly affected by illegal substance abuse or withdrawal symptoms resulting from prenatal drug exposure)."
In 2019, only 5 states and 2 jurisdictions reported serving children determined eligible under an "at-risk" category, while other states may include risk factors within their diagnosed/established conditions list.
Each state determines its definition of "at-risk" and whether single or multiple risk factors are included in their at-risk definition. The at-risk eligibility category can be used to provide early intervention to young children and their families where there are family circumstances (for example, substance use disorder, domestic violence, homelessness, abuse, and neglect) that result in an increased risk of developmental delay, especially social-emotional delays.
Summary of IECMH Opportunities Regarding Screening, Assessment, and Eligibility
Based on the information in this section, state early intervention (Part C) programs should consider the following strategies related to "referral, screening, assessment and eligibility" that can help ensure the participation of children with social-emotional and mental health concerns in early intervention:
- Expand child find outreach efforts to the full range of providers and settings that serve children at-risk of social-emotional difficulties (for example, social service organizations, domestic violence or homeless shelters).
- Encourage other early learning and care providers (for example, home visiting, child care, Early Head Start) and healthcare providers to screen for social and emotional development concerns. The American Academy of Pediatrics and Bright Futures Recommendations for Preventive Pediatric Health Care periodicity chart includes psychosocial and behavioral screening beginning at birth.
- Partner with the child welfare agency to examine CAPTA and CARA Plans of Safe Care policies and procedures to ensure timely and effective referrals of children with potential social-emotional delay and mental health issues dues to maltreatment and/or parental abuse use in utero.
- Promote use of screening tools that address social and emotional development.
- Promote use of a tool focused on social and emotional development as part of the evaluation to supplement the multi-domain tool used.
- Promote the inclusion of a licensed mental health specialist or professional trained and/or endorsed in IMH on the evaluation team when appropriate (for example, CAPTA referrals, when there are social and emotional development concerns or family risk factors), who may either be a member of the early intervention team or accessed through a partnership with another agency.
- Expand the list of diagnosed conditions for eligibility to include additional IECMH-related conditions including attachment disorder, posttraumatic stress, trauma, depressive and other mood disorders, eating, sleep, crying, and regulation disorders.
- Partner with other organizations to provide training for mental health clinicians to help identify the presence of infant mental health conditions (for example, DC:0–5) that can also help teams determine whether the child and family could benefit from a referral for evidence-based IECMH intervention or treatment.
Services and Practices

This section addresses IECMH services and practices to incorporate into early intervention (Part C) or to access through partnerships and referrals. This section examines:
- IECMH Promotion — public awareness of the importance of social-emotional development and mental health needs of infants and toddlers;
- IECMH Prevention-Intervention — including Reflective Practice, FAN approach, IECMH consultation, Pyramid Model, NEAR@Home; and
- IECMH Treatment — parenting programs and dyadic treatment or therapy models.
IECMH Promotion
Public Awareness and Universal Professional Development
Early intervention (Part C) at the state and local level plays a role in helping early learning and care and the wider community understand the importance of healthy social-emotional development for infants and toddlers within the context of relationships with their parents and other important caregivers in the child's life.
State early intervention (Part C) programs can collaborate with other programs and organizations to develop public health campaigns, educational materials, and other efforts to help build public awareness of the importance of social and the emotional development and mental health needs of young children.
Early intervention (Part C) programs can also support the integration of IECMH-informed training into the initial and ongoing training for practitioners, supervisors, and administrators to increase their knowledge about how IECMH practices and services can promote healthy social and emotional development (see the Workforce Development section of this paper for more information regarding professional development opportunities).
ZERO TO THREE suggests that public awareness efforts include the following:
- Conduct public awareness campaigns to promote infants' and young children's positive social and emotional development and educate families at-risk about available supports.
- Develop parent educational materials for distribution by health care providers (for example, obstetricians, pediatricians, nurse practitioners, psychiatrists) highlighting ways parents can promote child well-being through everyday moments, care for their own mental health, recognize signs of maternal depression, and identify community resources for help.
- Distribute parent education materials through public benefit programs (for example, WIC).
- Encourage public-private partnerships with local foundations to support IECMH efforts.
- Host learning collaboratives for stakeholders (including providers and payors) to share best practices and address barriers in advancing the State's IECMH goals.
IECMH Preventive-Intervention
IECMH preventive-intervention practices can be used by practitioners to support healthy parent-child relationships to prevent severe relationship and mental health issues, but also provide a foundation from which parents can nurture and promote their child's development across domains.
The following IECMH practices can be used by intervention providers from across disciplines, not just mental health professionals on the team. These practices can be incorporated into professional development either as distinct trainings or threaded into existing training modules (see the Workforce Development section later in this document).
Preventive-intervention approaches and their requirements for personnel qualifications and training/certification are presented in Figure 10.
Figure 10. Preventive Intervention Approaches and Models
| Approach/Model | Required Qualifications | Training/Certification |
|---|---|---|
| Reflective Practice (see Workforce Development section for Reflective Supervision/Consultation) | No minimum qualifications — all professional disciplines. | No formal training/certification required. |
| Facilitating Attuned Interactions (FAN) | No minimum qualifications — all professional disciplines. | Typically 3 days, and 6-9 months of mentoring/coaching and booster training. Train-the-trainer available. |
| IECMH Consultation | Varies by state and program — typically Master's degree in mental health or related field. May require endorsement. | Varies by state and program. |
| Pyramid Model | No minimum qualifications — all professional disciplines. | NCPMI supports states with implementation, including modules and coaching with tools and videos. |
| NEAR@Home | No minimum qualifications — all professional disciplines. | Facilitated learning, including reflective consultation. |
Reflective Practice
Early intervention (Part C) practitioners can incorporate "reflective practice" in their work with all children and families. Reflection is a core IECMH competency that includes "contemplation, self-awareness, curiosity, professional/personal development, parallel process, and emotional response", and the capacity to "hold others' minds in mind, as well as one's own" (Michigan Association for Infant Mental Health, 2017, p.38).
The Workforce Development section of this document for how reflective supervision/consultation (RS/C) can be used to support individuals practitoners or groups of practitioners to reflect on their work.
The New York State Association for Infant Mental Health provides the following definition:
"Reflective practice is at the heart of working with and caring for infants, young children and their families… Reflection involves the process of considering multiple perspectives including cognitive, relational, emotional, development, and cultural. It requires stepping away from the work to consider one's own thoughts and feelings, as well as the experiences of the caregiver and infant."
ZERO TO THREE provides another helpful definition:
"Reflection means stepping back from the immediate, intense experience of hands-on work and taking the time to wonder what the experience really means. What does it tell us about the family? About ourselves? Through reflection, we can examine our thoughts and feelings about the experience and identify the interventions that best meet the family's goals for self-sufficiency, growth, and development."
In addition to reflection with a trained reflective supervisor or consultant, early intervention professionals may also practice ongoing "self-reflection", regarding their work with infants, toddlers, and their families.
This can include taking time after a home visit to reflect on their interaction with the family and the parent's interaction with their infant/toddler. Such reflective practice includes "wondering" and "remaining open and curious" about emotions the child and the parent may be feeling about the visit as well as reflecting on their own emotions and their own feelings and emotions as the practitioner. Self-reflection strategies include jotting down feelings and thoughts in a journal or recording a voice memo on the phone, to address later in reflective supervision/consultation.
Facilitating Attuned Interactions (FAN)
The Facilitating Attuned Interactions (FAN) approach, developed by Linda Gilkerson, PhD and colleagues with the Fussy Baby Network at the Erikson Institute, is both a conceptual model and a practical tool for family engagement and reflective practice.
The FAN approach helps practitioners:
- improve their ability to read parents' cues and respond with interventions that match what parents need moment-to-moment;
- recognize and regulate their own feelings when working with families to build their reflective capacity;
- improve the relationship they have with harder-to-engage families; and
- enhance their ability to provide attuned developmental information in a way that increases parental capacity.
For early intervention teams the FAN approach "may help increase collaboration with parents by shifting the mindset of the professional and facilitating more meaningful relationships with parents that enhance their child's ability to support their child's growth and development" (Cosgrove et al., 2019, p.254).
The FAN tool, shown in Figure 11, can help early intervention professionals read cues from parents and themselves and, thus, provide empathetic and appropriate responses.
For more information, see Wisconsin in Appendix A: State Spotlights.
Figure 11. Facilitating Attuned Interactions Tool (FAN)
Copyright © Gilkerson, 2016. Used with permission.
IECMH Consultation

IECMH Consultation (IECMHC) is a preventive service used to improve children's social-emotional development and behavioral health (ZERO TO THREE, 2017). According to The Center of Excellence for Infant and Early Childhood Mental Health, the aim of IECMH consultation is to build adults' capacity to strengthen and support the healthy social and emotional development of children.
IECMHC is rooted in relationship-based practice that recognizes the importance of strong, positive relationships between the practitioner and parents/caregivers to support effective caregiving practices that promote young children's development. Consultation is individualized to address the immediate needs of a child, family, and program.
While IECMHC has helped early childhood educators meet the social, emotional, and mental health needs of young children in classroom settings, more recently it has expanded into other settings such as primary care, child welfare, home visiting programs, and early intervention.
IECMH consultants, in collaboration with the early intervention practitioner, explore strategies to address the mental health needs of children, families, and staff. They can also help the team determine when a referral for IECMH treatment is recommended to help restore or create a healthy and nurturing parent-child attachment relationship, often earlier and before a child exhibits more extreme issues that require more intensive intervention or treatment.
For more information, see Alabama in Appendix A: State Spotlights.
In addition to working with individual early intervention practitioners and teams, IECMH consultants can also help local early intervention programs build the capacity of their early intervention personnel to support the social, emotional, and mental health needs of the children, families, and staff. General topics and/or themes include working with families that have many challenges, working with resistance, understanding parental depression, etc. IECMH consultants can provide "programmatic" consultation for administrators, such as to consider the impact policies and procedures may have on family engagement, relationships among staff and families, etc. (Center of Excellence for Infant and Early Childhood Mental Health, 2020).
IECMH consultants may work for early intervention programs as staff, contractors, or for a local or regional organization that provides IECMH consultation to home visiting, child care, Pre-K, Head Start or Early Head Start as part of collaborative efforts.
For more information, see Illinois in Appendix A: State Spotlights.
Pyramid Model for Promoting Social and Emotional Competence in Infants and Young Children
The Pyramid Model for Promoting Social Emotional Competence in Infants and Young Children promotes social-emotional development, supporting children in experiencing responsive relationships with caregivers, developing relationships, exploring and learning within environments, communicating in play, and expressing and regulating emotions.
The Pyramid Model's tiered promotion-prevention-intervention approach includes universal practices to promote social-emotional development, secondary prevention practices to address the needs of children with social-emotional delays, and intensive individualized interventions for children with persistent challenging behavior — all supported by an effective workforce (see Figure 12).
The Pyramid Model framework is used within early intervention services, infant-toddler care environments, family child care homes, early childhood programs, Head Start, and public early childhood education programs. The National Center for Pyramid Model Innovations (NCPMI) provides materials, resources, and technical assistance for using the Pyramid Model in Part C early intervention programs.
Figure 12. Pyramid Model Tiers
NCPMI promotes the following primary principles for using the Pyramid Model with infants and toddlers and their families in early intervention (Part C):
- Support practitioners in building collaborative partnerships with all families.
- Use family coaching strategies to meet the needs of all caregivers.
- Provide families with knowledge and skills related to responsive caregiving and nurturing and responsive relationships.
- Build families' confidence and competence in supporting their child's social-emotional development.
- Provide families with tools and strategies that address and focus on the prevention of challenging behavior.
NCPMI provides resources for the program-wide implementation of Pyramid Model practices in early intervention Part C. These materials include:
- Roadmap to Effective Intervention Practices: Statewide Implementation of the Pyramid Model and State Leadership Team Benchmarks of Quality: Implementing the Pyramid Model Statewide — materials state teams use to guide widespread implementation of the Pyramid Model;
- Pyramid Model Training for early intervention service professionals;
- Pyramid Model Early Intervention (Part C) Benchmarks of Quality: fidelity tool program or agency leadership teams use to guide implementation of critical elements of the approach;
- Early Interventionist Pyramid Practices Fidelity Instrument (EIPPFI) — fidelity tool early interventionists and coaches use to assess practice strengths and identify areas for growth. Practice domains of the EIPPFI are:
- building partnerships with families;
- social-emotional development;
- family-centered coaching;
- dyadic relationships;
- supporting families with children with severe, persistent challenging behavior; and
- social-emotional assessment.
- early intervention practitioner coaching materials (for example, coaching guidance, strategies, and log); and
- early interventionist practice implementation materials (for example, practice checklist, caregiver practices, family-centered coaching strategies).
NCPMI includes resources that address the relationship between the Pyramid Model and Early Childhood Mental Health Consultation and include a Crosswalk of Infant Early Childhood Mental Health Consultation and Pyramid Model Coaching. These resources examine how partnerships with IECMH consultants can support Pyramid Model implementation through consultation to the program leadership team, consultation to practitioners, and guiding the provision of supports and services to children and their families.
They also examine how IECMH consultants can bring additional expertise to the Pyramid Model framework, for example:
- considering trauma-informed care;
- attachment to caregivers;
- supporting staff and families experiencing depression or adversity; and
- working with families where members with substance use disorder.

For more information, see Nevada in Appendix A: State Spotlights.
NEAR@Home
NEAR@Home is a home visiting approach developed by Start Early (formally Ounce of Prevention) that incorporates neuroscience, epigenetics, Adverse Childhood Experiences (ACEs) Study, and resilience.
The NEAR@Home Toolkit: A Guided Process to Talk About Trauma and Resilience in Home Visiting includes resources that incorporate the core elements for effective home visits to help strengthen families: preparing, asking, listening, accepting and affirming, and remembering and following up incorporates reflective supervision and a trauma-sensitive approach. The approach has been used in home visiting, but is also applicable to early intervention.
Figure 13. NEAR@Home Theory of Change
Home Visiting Systems and Leaders…
- …are knowledgeable and committed to bringing NEAR into home visiting.
- …support home visitors and home visiting supervisors with quality reflective supervision.
Home Visitors…
- …are supported by leadership that is knowledgeable and committed to bringing NEAR into home visiting.
- …are supported by quality reflective supervision, and their supervisors are supported by quality reflective supervision.
Parents…
- …deserve to know about the most powerful determinant of public health.
- …have a chance to talk about how ACEs have affected their lives in the context of a safe and respectful relationship.
- …have an opportunity for a change moment: the experience of feeling heard, understood, and accepted.
- …make decisions, and are able to take actions in their lives that protect their children.
- …engage with community and professional supports to develop parenting skills, manage stress, and build resilience.
- …take steps to develop their capacity to be sensitive and responsive to their children.
Children…
- …have fewer ACEs and more resilience than prior generations.
IECMH Treatment
IECMH treatment can help infants and young children and their families for whom the parent-child relationship has been significantly disrupted.
According to the Handbook of Infant Mental Health, there have been "dramatic advances in the knowledge base of infant mental health… perhaps none is as striking as the growing evidence base about effective interventions" (Zeanah, 2019, p.481).
Extreme disruption includes experiences of trauma, such as abuse or neglect of the child or siblings, interpersonal/domestic violence, mental health or substance use disorder affecting parenting ability, etc.
Disruption can also happen when parents' own experience of childhood trauma affects their ability to parent or when parents struggle to accept having a child with a disability. Referral for IECMH treatment may also include children with a diagnosed mental health disorder.
The early intervention team in collaboration with an IECMH consultant or mental health professional can determine whether a referral for IECMH treatment is recommended.
Parenting Programs
Parenting programs can be considered both preventive-intervention and treatment services. They can be used with families experiencing parenting challenges and identified as potentially benefiting from participating in such programs.
These parenting group models have a strong focus on parenting skills and promotion of healthy parent-child relationships and positive social-emotional outcomes for children and often take place over several weeks.
According to the National Center for Children in Poverty (NCCP) national survey (Smith et al., 2020) 34 state early intervention (Part C) programs reported either providing or referring families to evidence-based and research-informed parenting group models provided by other organizations.
Most state early intervention programs offering parenting programs do not require or recommend a specific evidence-based model. States use a variety of funding sources to provide such parenting programs or the IFSP team may refer parents to a program offered by another organization. The parenting program can be listed as an "other service" on the IFSP.
Some examples of evidence-based parenting programs are included in Figure 14.
Figure 14. Evidence-Based Parenting Programs
- Circle of Security is a parenting program that promotes secure attachment in the parent-child relationship and uses video and graphics through 8-10 weekly sessions by a trained non-licensed facilitator. The Circle of Security-intensive includes group sessions over 6 months facilitated by a licensed clinician.
- Triple P — Positive Parenting Program has been developed over 35 years and implemented in more than 30 countries. Triple P can be used with parents of children birth-12 years and gives parents tools and strategies to raise their child in an environment that is safe, loving, and predictable, and gives parents the confidence and skills to build good relationships with their children.
- Incredible Years promotes emotional and social competence to prevent, reduce, and treat aggression and emotional problems in young children birth to 12 years old. The basic training for parent of infant occurs over 8-9 sessions and 12 sessions for parents of toddlers.
Dyadic Treatment and Therapy

Dyadic treatment/therapy aims to increase sensitive, responsive parenting, a healthy parent-child relationship, and positive child behavior and development.
In dyadic treatment, a clinician works with the infant or young child and parent together, partnering with the parent to notice the child's cues and to respond in ways that promote a strong, nurturing parent-child relationship through enjoyable interactions.
Some models address issues related to attachment, separation, trauma, and unresolved grief and loss as they affect the care of the infant or toddler.
The National Center for Children in Poverty (NCCP)'s PRiSM page on Dyadic Treatment describes several models that have shown evidence of effectiveness in treating social-emotional, mental health, and behavioral problems in young children. These evidence-based treatment therapies involve rigorous training and certification for clinicians and may have qualification, licensure, or endorsement requirements.
In 2020, 24 state early intervention (Part C) programs reported providing dyadic treatment to eligible infants and toddlers and their families according to the NCCP's 50 state survey with six states requiring and another six states recommending the use of particular evidence-based models (Smith et al., 2020).
Several states are engaged in efforts to train clinicians in evidence-based dyadic treatment to expand the number of children and parents who can have access to this treatment. Other states may refer families to other community organizations or licensed mental health clinicians for dyadic treatment.
Figure 15 presents dyadic therapies applicable for children birth to three and their parents, according to PRiSM, that are considered either evidence-based practices (EBPs) or promising practices (PPs).
For more information, see Georgia in Appendix A: State Spotlights.
Figure 15. Dyadic Treatments and Therapies
Evidence-Based Practices (EBPs)
- Child-Parent Psychotherapy (CPP) is for children from birth to five years who have experienced trauma or are at-risk of insecure attachment or social-emotional problems. Randomized controlled trials have shown significant improvements in children's mood, challenging behaviors; trauma symptoms and biological stress response (cortisol) and improvements in parent's mood, stress, trauma symptoms and parental relationship, as well as improvements in parent-child relationship quality.
- Parent-Child Interaction Therapy (PCIT) involves observation and coaching of parent-child interactions to address challenging behavior for children from two to seven years. Several studies have examined PCIT effectiveness that conclude that this dyadic treatment reduces child behavior and parent stress and improves parent-child interactions among children with behavior scores in the clinical range.
- Attachment and Biobehavioral Catch-up (ABC) is a 10-week in-home program to help parents provide nurturing care to children from 6 to 24 months old who have experienced early adversity. ABC providers coach parents and other caregivers during in-person sessions in practices that help children develop attachment, self-regulation, and coping skills. A systematic review of randomized control trials of ABC conducted with populations of children involved in child welfare or foster care found that the program had positive impacts across several child outcomes, including fewer problem behaviors, and greater positive attachment.
Promising Practices (PPs)
- Parent-Child Care (PC-CARE) is a six-week dyadic treatment program for children ages 1-10 and their parents or caregivers who have experienced trauma. With fewer sessions than traditional therapy models, it has been found to improve children's behavior, improve parenting, and reduce parenting stress.
- Infant Mental Health Home Visiting (IMH HV) is a dyadic treatment model in which licensed mental health professionals provide infant-parent psychotherapy, developmental guidance, emotional support, etc., using a home-based approach. IMH HV has been in use in Michigan for more than 40 years with an evaluation underway to assess the impact.
Summary of IECMH Opportunities Regarding Services and Practices
Based on the information provided in this section, we believe state early intervention (Part C) systems should consider increasing access to IECMH services and practices, as follows:
- Promote a focus on the importance of the social and emotional development and mental health of infants and toddlers within the context of relationships through a collaborative public awareness campaign.
- Promote a basic understanding of IECMH and prevention and intervention practices that support healthy social and emotional development and parent-child relationships through professional development and guidance materials for early intervention practitioners, supervisors, and administrators.
- Support implementation of preventive-intervention models/approaches (for example, reflective practice, FAN Approach; Pyramid Model; NEAR@Home) utilizing implementation science strategies (for example, professional development, coaching and supporting leadership).
- Develop a system of IECMH consultation to support early intervention practitioners in identifying and better meeting the social-emotional needs of eligible infants and toddlers with mental health needs and supporting the parent-child relationship. This may be accomplished in collaboration with other early learning and care or mental health agencies or organizations.
- Encourage relationships at the local level between early intervention (Part C) and local mental health professionals and organizations, such as community mental health agencies, local early childhood coalitions/groups, and associations of infant mental health to facilitate coordination of services.
- Support access to evidence-based dyadic treatment when the parent-child relationship has been negatively affected by trauma or other family stressors. Clinicians trained in these approaches may be a part of early intervention teams or accessed through another program/organization.
- Support access to evidence-based parenting programs that focus on positive parent-child relationships and parenting skills to promote the child's social-emotional growth.
- Encourage early intervention teams to help adult family members access needed mental health, including supports (for example, screening, evaluation, and treatment for mental health needs including post-partum depression, substance use disorder, and access to needed domestic violence support) that present challenges to the parent-child relationship.
Workforce Development

This section addresses how state early intervention (Part C) programs can support early intervention professionals in the use of effective IECMH practices, including:
- Competencies — incorporating IECMH into competencies for early intervention (Part C) certification and/or in professional development;
- Professional development — incorporating IECMH practices into existing training and coaching, as well as developing/supporting specific IECMH training;
- Endorsement — encouraging infant mental health endorsement (if available); and
- Reflective supervision — supporting and promoting reflective supervision for early intervention practitioners.
Competencies

Personnel competencies or standards describe the knowledge, skills, and disposition of a professional discipline. Personnel competencies or standards differ from state licensing or certification issued by state or national agencies to individuals who meet specific requirements, such as graduation from an accredited Institution of Higher Education (IHE) program, or passing a national examination.
As such, they guide state certification and licensing requirements for each specific professional discipline and guide curriculum development for IHE professional preparation programs and in-service professional development (Bruder et al., 2019).
Some state early intervention (Part C) programs have developed specific early intervention competencies as part of certification for developmental specialists (special educators) and to guide professional development. These state competencies may be based on or include:
- The Division of Early Childhood (DEC) has both Initial Practice-Based Standards for Early Interventionists/Early Childhood Special Educators and Recommended Practices for early intervention that support young children's access and participation in inclusive settings and natural environments.
- Early Childhood Personnel Center (ECPC), an Office of Special Education Programs (OSEP) funded project that has developed Cross-Disciplinary Competencies for early intervention that incorporate family-centered practices that "support families in their caregiving role of [with] their child".
- The ZERO TO THREE Competencies for Prenatal to Age 5 (P-5) include specific evidence-based teaching methods and practices that support and nurture young children's social-emotional, cognitive, and language and literacy development and learning.
State competency systems may include using Practice-Based Coaching to support the acquisition of competencies of key practices and to promote the fidelity of evidence-based practices. This may include observation of the practice being performed, either in-person or a recording of the early intervention visit together with structured coaching sessions.
Specific IMH competencies were first developed by the Michigan Association for Infant Mental Health (MI-AIMH). The Michigan Department of Education (MDE), the lead agency for early intervention (Part C), recognized that "infant mental health is a specialization within the early intervention field" and supported a cross-disciplinary group of experts to develop competencies that were approved by the MI-AIMH board in 1997 (Michigan Association for Infant Mental Health, 2017, p.5). The IMH competencies are built on those identified in the MI-AIMH Training Guidelines (1986) along with the TASK Documents published by ZERO TO THREE in 1990, and early intervention competencies developed by the MDE in 1996.
The eight competency areas have been further refined over the years to include:
- theoretical foundations;
- law, regulation, and agency policy;
- systems expertise;
- direct service skills;
- working with others;
- communicating;
- thinking; and
- reflection.
These IMH competencies apply to all infant and family-serving disciplines, sectors, and scopes of practice. Because they are based on competencies created specifically for early intervention, they can be particularly helpful for the early intervention Part C workforce. They provide a framework for individuals and systems to identify existing areas of competence (for example, infant development, disorders of infancy, family-centered practice, screening and assessment) and areas where additional training may be required (for example, relationship-based practice, attachment, trauma, grief, and loss).
The Alliance for the Advancement of Infant Mental Health licenses the use of the Competency Guidelines and/or Endorsement for Culturally Sensitive, Relationship-Focused Practice Promoting Infant & Early Childhood Mental Health to state associations of infant mental health (AIMHs) that have been established in 33 states.
Some states, such as California, have developed their own competencies. The California Center for Infant-Family and Early Childhood Mental Health produced a California Compendium of Training Guidelines, Personnel Competencies, and Professional Endorsement Criteria for Infant-Family and Early Childhood Mental Health, which ties personnel competencies to endorsement and training for professionals working with young children and their families across the continuum of infant-family and early childhood mental health.
The Center of Excellence for Infant and Early Childhood Mental Health Consultation Competencies describe "building a national consensus on the knowledge and the array of foundational skills and abilities needed to become a competent IECMH consultant".
State early intervention (Part C) programs may consider incorporating IECMH competencies into their competencies or personnel standards.
For more information, see North Carolina in Appendix A: State Spotlights.
Professional Development

IDEA Regulations 34 CFR §303.118 require state early intervention programs to establish and maintain a Comprehensive System of Personnel Development (CSPD) that includes the training of early intervention personnel, promoting the higher education preparation of students to enter the early intervention field, and establish requirements for qualified personnel in 34 CFR §303.31.
Several state early intervention (Part C) programs partner and fund universities or other organizations to provide in-service training and other professional development. Some states tie training requirements to certification of early intervention practitioners, with some states requiring continuing education to maintain a practitioner's certification.
State early intervention (Part C) programs should explore how to incorporate IECMH prevention and preventive-intervention practices into a variety of professional development opportunities for all early intervention practitioners. Additionally, states may also target specific professional development to mental health professionals, for example, social workers, family therapists, and psychologists for evidence-based treatments.
Professional development for all early intervention personnel may include, but is not limited to:
- the science of early relationships for healthy social emotional development for infants and toddlers (for example, Introduction to Attachment Theory);
- reflective and relationship-based practices;
- trauma-informed care to address ACEs (Adverse Childhood Experiences);
- Reflective Supervision/Consultation (RS/C) inclusive of supervisors and administrators, in addition to practitioners who will receive RS/C;
- how to write functional IFSP outcomes and strategies that address the social and emotional needs of children and family outcomes and may include IECMH treatment;
- training and ongoing opportunities for building self-awareness (for example, through RS/C); and
- learning about local community agencies or resources that are available as supports to families when additional IECMH services are needed.
Training on particular models or approaches can also be offered to early intervention practitioners, including:
- The Pyramid Model Consortium's Pyramid Model Practices;
- Center of Excellence for Infant and Early Childhood Mental Health's IECMH Consultation;
- Erikson Institute's Facilitating Attuned Interactions Approach (FAN); and
- Start Early's NEAR@Home.
Training on treatment-level IECMH models and approaches may also be offered to mental health clinicians in collaboration with other early childhood agencies and organizations, such as state children's mental health agencies, local community mental health agencies, and associations of IMH (if operating in their state). Specialized training in evidence-based dyadic treatment can be conducted collaboratively across state agencies and even across states.
States may consider establishing Communities of Practice to support practitioners interested in using IECMH practices within early intervention (Part C). At the national level the Division of Early Childhood (DEC) has established an Infant Mental Health Community of Practice to build the capacity of early intervention professionals around IECMH topics, increase knowledge of IECMH topics within local communities (including parents), support Institutes of Higher Education to provide courses and/or certification related to IECMH, increase awareness of and advocate for IECMH within local/state agencies, and explore funding opportunities for IECMH activities.

For more information, see Georgia in Appendix A: State Spotlights.
Endorsement
Endorsement is a credential that recognizes experiences that lead to competency. It does not replace licensure or certification but is meant as evidence of a specialization in IECMH. Endorsement can be cross-sector and multidisciplinary, recognizing a professional from any of several professional backgrounds (for example, counseling early childhood and special education, nursing, pediatrics, psychiatry, psychology, social work) who have "completed specialized education, work, in-service training, and reflective supervision/consultation experiences that have led to competency in the promotion and/or practice of infant mental health" (Michigan Association for Infant Mental Health, 2017).
The Alliance for the Advancement of Infant Mental Health includes four Pathways to Early Childhood Mental Health Endorsement that are issued by state associations of IMH to professionals who are working with young children and families that apply.
These pathways include the specific work, education, in-service training, and reflective supervision/consultation requirements as well as the competencies for each of the four roles shown in Figure 16.
The National Center for Children in Poverty (NCCP) national survey of early intervention (Part C) states found that some states are working with their state's AIMH to offer training and IECMH endorsement to early intervention providers (Smith et al., 2020).
State early intervention (Part C) programs can support and encourage early intervention practitioners and particularly mental health clinicians to pursue IMH endorsement, if available through their state association of IMH or where states have their own IMH endorsement system (for example, California, Illinois).
Figure 16. Pathways to Infant Mental Health Endorsement
| IMH Endorsement Level | Scope of Practice |
|---|---|
| Infant Family Associate (IFA) | IMH promotion |
| Infant Family Specialist (IFS) | IMH prevention/early intervention |
| Infant Mental Health Specialist (IMHS) | IMH treatment |
| Infant Mental Health Mentor (IMHM) | Leadership:
|
Reflective Supervision/Consultation (RS/C)

Reflective supervision has been characterized as a "relationship for learning" (Heller & Gilkerson, 2009, p.7) and "the process of examining, with someone else, the thoughts, feelings, actions, and reactions evoked in the course of working closely with infants, young children and their families" (Eggbeer et al., 2007, p.5).
Others have written that reflective supervision, "When it's going well… is a holding environment, a place to feel secure enough to expose insecurities, mistakes, questions and differences" (Fenichel, 1992, p.37), and "A safe, trusting reflective supervisory relationship, trusting reflective supervisory relationship develops most optimally with opportunity for regularly scheduled meetings between supervisor and supervisee(s) at a consistent time that is mutually agreed on, in a place that is comfortable, protected, and free from distractions or interruptions" (Weatherston & Eidson, 2019).
The term Reflective Supervision/Consultation (RS/C) is used to recognize that reflective support may come from a supervisor or a consultant from outside the agency. Regular and ongoing RS/C can be conducted with individual practitioners and with groups.
In an earlier section of this paper, we addressed reflective practice as a key strategy for early intervention practitioners to use to examine their thoughts, feelings and behaviors in their ongoing work with infants, toddlers and their families. RS/C provides an ongoing, regularly scheduled, and safe environment to do that reflection and provides support to the practitioner and can lead to professional growth and improve practice.
The University of Minnesota Center for Early Education and Development (CEED) identifies the key elements of reflective supervision as:
- Regularity: Committing to a protected, consistent, regularly scheduled meeting time
- Reflection: stepping back from the experience to sort through feelings and thoughts about what one is observing and doing.
- Collaboration: working together as a partnership in which control of power is shared, rather than an expert/learner dynamic.
CEED studied the impact of reflective supervision with a cross-disciplinary group of early childhood professionals who received monthly group reflective supervision which led to the development of the "4Rs" Model:
- Release: RS/C provides an outlet for participants to release the mental and emotional stress that builds up while working directly with highly stressed families and young children. Participants were able to voice concerns and frustrations and receive validation and affirmation. The experience of being held safely in the relationships within their group acted as a safety valve, so they could let go of the strong emotions that arose from their work.
- Reframe: Participating in safe relationships allowed practitioners to ask themselves questions about their work, consider multiple perspectives, and unpack their own assumptions. These processes were critical to understanding family context and seeing clients from a strengths-based perspective.
- Refocus: RS/C helped practitioners distill the areas of their work where they believed they could have the most impact despite the multiple stressors facing each family. It helped them think of new ways to approach their work and reduced feelings of helplessness and hopelessness.
- Respond: Participating in RS/C helped practitioners slow down and become more flexible in their work. They reported becoming more responsive to families' needs rather than their own fixed agenda. They were able to purposefully create the safe, trusting relationships with families necessary for their work.
Keys to meaningful engagement in reflective supervision and to deepen one's reflective capacity include building trust, emotional regulation, curiosity, bravery, self-awareness, and vulnerability. These skills also help one examine one's own values and perspective, which can deepen reflection and lead to personal and systematic action and change.
Summary of IECMH Opportunities Regarding Workforce Development
Based on the information provided in this section regarding IECMH workforce development we believe state early intervention (Part C) programs should consider the following opportunities, which may be addressed through collaborative partnerships with other organizations/agencies:
- Incorporate IECMH topics into training modules for all early intervention practitioners, supervisors and administrators, including ACEs, toxic stress and the critical importance of early relationships for healthy social-emotional development and mental health of young children.
- Make training available to EI practitioners on preventive-intervention models/approaches (for example, FAN Approach; Pyramid Model; NEAR@Home) and reflective practice.
- Make training available to mental health clinicians on evidence-based parenting groups and dyadic treatments.
- Incorporate IMH competencies into state early intervention competencies, where applicable.
- Promote and encourage mental health professionals (for example, counselors, social workers, psychologists) in early intervention to receive IECMH training and/or endorsement as Infant Mental Health Specialist (IMHS) category or Infant Mental Health Mentor-Clinical.
- Promote and encourage some early intervention practitioners to become endorsed at the Infant Family Specialist (IFS) category.
- Support the development of an infrastructure system of reflective supervision/consultation (RS/C) to allow all early intervention personnel to receive regular and ongoing reflective supervision.
Funding, Partnership, and Collaboration

This section examines funding opportunities that state early intervention (Part C) programs may use to promote and make available IECMH services and practices, including:
- funding for IECMH services through existing funding for EI services;
- partnership and collaborations; and
- federal and philanthropic grants.
State early intervention (Part C) programs use a variety of funding sources to fund direct services and system functions (for example, professional development, general supervision/accountability) including federal IDEA Part C grant funds, Medicaid, private insurance, state allocations and family fees and local funds (IDEA Infant & Toddler Coordinators Association, 2018).
IECMH Services Funded As Part of the IFSP
The following early intervention services under the IDEA Regulations 34 CFR §303.13 can be seen as allowing for the provision of IECMH services:
- Family training, counseling, and home visits include counseling by social workers, psychologists, and other qualified personnel (for example, family therapists) (34 CFR §303.13(b)(3) and 34 CFR §303.13(c)).
- Psychological services include obtaining, integrating, and interpreting information about child behavior and child and family conditions related to learning, mental health, and development, and also psychological counseling for children and parents and family counseling (34 CFR §303.13(b)(10)).
- Social work services include social or emotional developmental assessment of the infant or toddler within the family context and Providing individual and family-group counseling with parents and other family members, and appropriate social skill-building activities with the infant or toddler and parents (34 CFR §303.13(b)(13)).
34 CFR §303.13(d) clarifies that nothing prohibits the identification in the IFSP of another type of service as an early intervention service, provided that the service meets the criteria identified in 34 CFR §303.13(a).
Therefore, IECMH services can be provided as part of the IFSP if they are designed to meet the developmental needs of an infant or toddler with a disability and the needs of the family to assist appropriately in the infant's or toddler's development (34 CFR §303.13(a)(4)), and are selected in collaboration with the parents (34 CFR §303.13(a)(2)).
As state early intervention (Part C) programs currently fund family counseling, psychological and social work services that are included in the IFSP, they can be used to provide and fund IECMH services and approaches by qualified personnel.
IECMH services can be provided and funded by another organization/agency and aligned and coordinated with other early intervention services on an IFSP, with all practitioners working as a transdisciplinary team. For example, a family may attend a parenting group or receive dyadic therapy that is provided and funded by another community organization.
Medicaid
All state early intervention (Part C) programs use Medicaid funding. However, the extent to which Medicaid supports the full range of early intervention services for children enrolled in Medicaid and early intervention (Part C) varies by state in both policy and practice.
Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) emphasizes prevention and early detection within its broad treatment mandate and can be used to fund early intervention services regardless of where early intervention (Part C) services are detailed in the Medicaid state plan that each state is required to submit to the US Centers for Medicare & Medicaid Services (Mann et al., 2019).
Federal Medicaid pays between 50% and 78% of the cost of services based on the current Federal Medical Assistance Percentage (FMAP) with states responsible for the remaining or "match" (Kaiser Commission on Medicaid and the Uninsured, 2012; Kaiser Family Foundation, n.d.). It therefore makes sense for state early intervention (Part C) programs to maximize the early intervention services funded through Medicaid for children enrolled.
IECMH Coverage Under Medicaid

Statutory clarifications, federal guidance, and legal decisions against state Medicaid programs have reinforced the inclusion of mental health services under EPSDT (Burak & Rolfes-Haase, 2018). A growing number of states have taken steps to add, identify, or clarify reimbursement for IECMH services (Smith et al., 2020).
Some states use Medicaid to pay for at least some mental health services in early intervention. A finance survey in 2018 found a majority of state early intervention (Part C) programs reported that their state used Medicaid to reimburse for family training/counseling (26 states), social work (25 states) and psychological services (29 states) (IDEA Infant & Toddler Coordinators Association, 2018).
Another survey by the National Center for Children in Poverty (NCCP 2018) on how states use Medicaid to cover IECMH services found that 35 states reported that Medicaid pays for an early childhood mental health specialist to provide services to address a child's mental health. The report found that 32 states use Medicaid to cover IECMH treatment (groups and dyadic treatment), with 15 states requiring the use of evidence-based tools or practices (Smith et al., 2018).
While IECMH intervention/treatment services can be funded by Medicaid, indirect services including IECMH consultation are less often funded through Medicaid since they are not tied to the individual service needs of a Medicaid-enrolled child. In 2018, 13 states reported that Medicaid funding is used for consultation with early childhood professionals and supports to address an individual child's behavioral and mental health needs (Smith et al., 2018). However, no states reported Medicaid funding for consultation with early childhood professionals and directors to help strengthen practices that promote young children's mental health and social-emotional growth.
A potential option for funding IECMH services under the Children's Health Insurance Program (CHIP) allows states to use up to 10% of CHIP funding to implement health services initiatives (HSIs). In 2019, 24 states had instituted an HSI through a state plan amendment, with six of these amendments being for behavioral health services (Medicaid and CHIP Payment and Access Commission, 2019).
Medicaid Funding Structure and Methodology

State Medicaid agencies decide the funding structure and methodology, including fee-for-service, where the state directly reimburses providers for services provided, or through managed care organizations (MCOs), in which the state contracts with private health insurance plans with a capitated rate (set monthly/annual amount) per member.
Most children in the U.S. are served through MCO plans. However, some states have been able to "carve out" early intervention (and IDEA Part B special education and related services) from managed care to be funded on a fee-for-service basis and determine rates for reimbursement rather than being negotiated by the MCOs.
If billing under a fee-for-service basis, state early intervention (Part C) programs either use established service codes for each service, while other states developed a specific billing code for early intervention services (often with modifiers for location or method—group or individual) with all disciplines billing under that code. That code can be used to bill for IECMH work conducted by a qualified practitioner (licensed social worker, counselor, family therapist, or psychologist). Alternatively, services provided by those disciplines can be billed under their distinct service codes.
Medicaid claims require a diagnosis code that is typically from the ICD-10 (International Classification of Diseases 10th Revision) and DSM-5 (Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition). Often a broad development delay (unspecified) code can be used. As discussed in the eligibility section, there are crosswalks from DC:0–5 to ICD-10 and DSM-5 that clinicians can use for IECMH conditions. Some state Medicaid agencies have begun to recognize or recommend the use of age-appropriate diagnostic tools for mental health, notably the use of DC:0–5 instead of the DSM-5 used for school-aged children and adults (Burak & Rolfes-Haase, 2018). State early intervention (Part C) programs should check with their state Medicaid partners as to whether DC:0–5 can be entered as the diagnosis code for billing or whether it needs to crosswalk to the applicable ICD-10 or DSM-5 code.
Some states have also used Z codes (social, economic, and environmental determinants known to affect health and health-related outcomes) to bill Medicaid when a developmental delay or diagnosed medical condition is not present.
Collaboration with Other Mental Health Agencies
State early intervention (Part C) programs may also collaborate closely with their state's children's mental health agency to ensure consistent processes and procedures for Medicaid services reimbursement for IECMH services.
Early intervention staff, along with their other mental health agency partners, can provide important expertise to state Medicaid officials on the social-emotional needs of young children and opportunities to prevent or mitigate more complex mental health challenges that can be more costly over time to encourage Medicaid funding of IECMH services.
While Medicaid is an important funding source for low-income families and children who may be eligible based on a disability diagnosis, states will also need to examine funding for IECMH services for other children and families, which may include private insurance, state IDEA Part C appropriations, and federal IDEA grant funds, which are seen as a payor of last resort.

For more information, see Hawaii in Appendix A: State Spotlights.
Partnerships and Collaboration
Provision of IECMH services (IECMH consultation, dyadic therapy, and parenting groups) or supports (Reflective Supervision/Consultation) may be achieved through partnerships and collaborations.
It may be possible for another agency or organization to provide and fund a service (for example, dyadic therapy may be funded through the state's child's mental health agency or parenting group funded through the child welfare agency, with additional slots funded by Part C).
Several states have convened collaborative IECMH initiatives/workgroups to explore and plan how states can provide a continuum of promotion, preventive-intervention, and treatment services for young children and their families. IECMH collaboratives can address how to braid funding sources both for services as well as how to jointly fund professional development opportunities across disciplines.
Institutionalizing partnerships and collaborations through an interagency agreement or memorandum of agreement/understanding can help ensure that the partnership continues regardless of leadership and agency changes. An interagency agreement can address shared funding and reduce duplication of efforts.
Federal and Philanthropic Grants
State early intervention (Part C) programs may also explore possible federal grants or philanthropic funding. Such grants rarely fund direct services but can be used to build IECMH infrastructure or systems.
This may include funding to study and make recommendations regarding state investments for IECMH services or funding for professional development to ensure that personnel are available to provide evidence-based services or funding for pilot programs, demonstration sites, and statewide systems building efforts.
Federal grants have included, for example, Linking Actions for Unmet Needs in Children's Health (Project LAUNCH) from the Substance Abuse and Mental Health Services Administration (SAMHSA) and early childhood infrastructure grants such as the Preschool Development Grant Birth through Five (PDG B-5) and the Race To the Top-Early Learning Challenge (RTT-ELC). The American Recovery Plan Act (ARPA) funds received by state early intervention (Part C) programs and other early childhood programs can also be used.
Summary of IECMH Opportunities Regarding Funding, Partnership, and Collaboration
Based on the information provided in this section, the following opportunities exist for state early intervention (Part C) systems about IECMH funding, partnership, and collaboration:
- Examine state policies, standards, regulations, service definitions, codes, and rates to determine the ability to bill for IECMH services as part of the IFSP.
- Meet with state Medicaid partners to examine Medicaid funding of IECMH services, including the use of applicable diagnosis codes.
- Collaborate with the state mental health and/or IECMH leaders to explore how IECMH services can be made available to families eligible for early intervention (Part C).
- Join or convene an IECMH collaborative workgroup with other agencies/organizations to explore braiding funding for IECMH services, professional development, and effective IECMH systems building.
- Explore federal or philanthropic funding opportunities for IECMH systems building, professional development, etc.
Implementation Strategies

This section examines potential strategies that state early intervention (Part C) programs can undertake to promote IECMH policies and practices over a period of several years, including:
- developing partnerships with state agencies and organizations and cross-agency/program IECMH initiatives;
- garnering support for IECMH efforts;
- examining possible next steps to move forward;
- utilizing implementation science; and
- data collection and analysis considerations.
Partnerships
State early intervention (Part C) programs can and should collaborate and partner with other agencies and organizations to implement IECMH policies and practices.
Potential Partners
State Associations for Infant Mental Health (AIMH)
33 state associations of infant mental health exist to support and promote professional development and endorsement of practitioners and licensed the use of the Competency Guidelines and/or the Endorsement for Culturally Sensitive, Relationship-Focused Practice Promoting Infant Mental Health. Each of them also offers interdisciplinary training that is competency-based and supports putting infant and early childhood principles into practice. Note: California Association for Infant Mental Health is not a member of the Alliance for the Advancement for Infant Mental Health.
State Children's Behavioral/Mental Health Agency
Each state has a designated agency to build and coordinate a system of care to meet the behavioral health needs of children and their families. The state children's behavioral/mental health agency is sometimes within the state Medicaid agency or in collaboration with Medicaid, as Medicaid is the largest funder of behavioral health services for children.
State IECMH Leadership
Several states, including Alabama, Georgia, New Mexico, and Michigan have funded a statewide IECMH lead/coordinator to facilitate and promote system and policy changes related to IECMH across state agencies and programs. These positions are located in various state agencies, including early learning and care or mental health agencies.
Universities and Colleges
University Centers of Excellence in Developmental Disabilities Education, Research, and Service (UCEDD) and other IHEs may provide cross-disciplinary programs to help professionals meet IECMH competencies.
Advocacy Organizations
Statewide advocacy organizations that focus on children and family or early childhood issues and policy issues may promote IECMH through public awareness campaigns.
Philanthropic Organizations
Statewide, regional, and or topic focused philanthropic organizations may be willing to partner to fund pilot projects, professional development, or IECMH collaborative initiatives.
Cross Agency and Program IECMH Initiatives
State early intervention (Part C) programs should determine if any of the following collaborative initiatives exist in their state and, if so, should partner with these initiatives to ensure that the needs and issues of early intervention are addressed. Collaborative initiatives include:
Cross-Agency/Cross-Program IECMH Initiatives
IECMH initiatives may focus on a particular policy or practice, such as promoting IECMH consultation, or may be a broader effort to build a statewide IECMH system across programs that serve young children and their families.
Pyramid Model
Several states have implemented the Pyramid Model across early learning and care programs statewide or within particular regions to promote evidence-based practices for social and emotional development and to help staff address challenging behaviors across programs. States establish a Pyramid Model Leadership Team, including representatives from administrators and practitioners from a variety of programs. The leadership team oversees development and roll-out across the state using data-based decision making and monitoring outcomes.
Garnering Support for IECMH Efforts
State early intervention (Part C) programs may consider the following to garner support for prioritizing efforts and expenditures to promote IECMH policies and practices:
Interagency Coordinating Council (ICC)
Meet with the state ICC to discuss and examine their support for a focused initiative around IECMH. Consider making a joint presentation with a state IECMH champion on the fundamentals of IECMH and its relevance to early intervention (Part C) and identify and discuss steps that the state early intervention program may take to promote IECMH. If the ICC has a subcommittee on effective services and practices, work with that committee before presenting to the full ICC. ICC endorsement for a focus on IECMH can help the early intervention (Part C) program allocate funding and human resources to institute IECMH policies and support the implementation of IECMH practices and services.
Strategic Plan
If the state early intervention (Part C) program has a strategic plan, promoting IECMH policies and practices can be incorporated into that plan with goals and strategies to be achieved over one to five years.
State Systematic Improvement Plan (SSIP)
Several states' SSIPs focus on evidence-based practices to improve social and emotional outcomes for children in early intervention (Part C). States may consider implementing evidence-based IECMH services that are highlighted in this paper to address the social and emotional development of infants and toddlers in the context of relationships with parents and other caregivers.
Self-Assessment
The IECMH and Early Intervention (Part C) Planning Tool (see Appendix B) can be used to examine IECMH policies and practices to address and prioritize. A self-assessment can help state early intervention (Part C) programs review their policies and practices against those outlined in this briefing paper, including eligibility and assessment, services and practices, workforce and professional development, and funding policies.
Possible Next Steps
Given the many competing priorities and accountability requirements that state early intervention (Part C) programs must address, they may consider the following next steps:
Immediate Opportunities
Determine if there are any "easy wins" that can be achieved with relatively little effort, for example, current training modules or future modules can be revised to include IECMH, IECMH specialists can provide the keynote at a conference or host a focused webinar, and guidance can be provided on topics such as the use of social-emotional screening or assessment tools without changes to state regulations or policies.
Assign an IECMH Leader or Champion
Explore whether a staff person at the state early intervention (Part C) program has an interest or passion regarding IECMH issues and support them to take a lead as a champion of IECMH efforts. This person can build connections with key agencies and organizations and potentially play an active role in the state's association for IMH. For state early intervention (Part C) programs where the lead agency staff is very small, an alternative could be to look for a champion from an organization the state contracts with for professional development (for example, through a university or other organization). A final option could be for the state early intervention (Part C) program to develop a contract with someone to lead the IECMH initiative.
Raise Awareness of IECMH through Professional Development
Raise awareness of IECMH through professional development Consider hosting, or cohosting with partners, IECMH professional development events for early intervention (Part C) leaders and practitioners such as a keynote and/or workshop at a state conference, hosting a webinar or webinar series on IECMH that can be recorded and made available asynchronously, and promoting training on IECMH offered by partner organizations.
For more information, see Connecticut in Appendix A: State Spotlights.
Utilizing Implementation Science
As state early intervention (Part C) programs consider beginning or furthering statewide efforts to promote IECMH policies and practices they should consider resources that address the effective implementation of evidence-based practices.
ECTA Center and NCPMI identify essential support structures shown to help put evidence-based practices into widespread use:
"The essential support structures provide the leadership, training, practice application, and documentation necessary for statewide implementation.
- The State Leadership Team is an interagency group responsible for planning and supervising the initiative. They ensure support and resources are available to implementation sites, so sites can implement selected evidence-based practices with fidelity.
- Program Implementation Coaches are training and technical assistance professionals who guide Program Leadership Team(s) to ensure high fidelity implementation of evidence-based practices.
- Each implementation site's Program Leadership Team guides implementation, coaching, family engagement, behavior support planning, and data decision-making.
- Implementation sites use the Data and Evaluation System to measure fidelity of evidence-based practice implementation and inform decisions of the Program and State Leadership Teams."
The guide goes on to describe the stages of effective implementation in a State Process Guide and Community Process Guide as circular and dynamic, not linear, and often occur simultaneously. These implementation stages include:
- Exploration and Planning: The purpose of this stage is to explore the need and select the innovation that will successfully address it. While current infrastructure and accessibility may not be sufficient, there is a plan to improve them so the innovation can be adopted. During this time, it is critical to share information and gather input from representatives of each level of the system to assure the fit and feasibility of the innovation. This is also essential to establishing trusting partnerships.
- Installation: Installation builds infrastructure and system capacity to support the innovation. The SLT and partners assess the requirements of the innovation and compare it to current infrastructure and capacity. A plan is built that strengthens the system for the upcoming changes. Training and coaching for the innovation and its initial use begins in Stage 3, Initial Implementation.
- Initial implementation: In this stage the innovation is implemented and locally tested. The Professional Development Network (PDN) of Program Implementation Coaches share progress, outcomes, concerns, and challenges with the SLT to determine whether the implementation plan may need to be adapted.
- Full Implementation, Scale-Up, and Sustainability: Full implementation integrates the innovation and its supportive infrastructure into organizational best practices and aligns new infrastructure across state, community, and program contexts. In this stage, conflicting and duplicative practices are discontinued or streamlined and expansion plans for staff at pilot sites are created. The SLTs, program implementation coaches, Community and Program leadership teams will continue monitoring the infrastructure, performance, feedback, and outcomes and making minor infrastructure adjustments. Information learned from demonstration sites and improvement cycles is used to onboard new implementation sites and develop sustainability and scale up plans.
Data Collection and Analysis Considerations
In implementing a statewide IECMH initiative, state early intervention (Part C) should consider the data and measurement implications.
This can include examining whether their current data system can collect information needed to generate reports that help them analyze the status and evaluate change over time. Data may include:
- Referrals — including the type of organization making the referral;
- Eligibility — including children with social and emotional developmental delay or mental health related diagnosed conditions;
- IFSP service and service provision — including family training and counseling, psychological services, and social work;
- IFSP Outcomes — related to social-emotional development and enhanced parent-child relationships and parenting;
- Workforce — Including qualified mental health professionals (social workers, psychologists, and family therapists), training modules/workshops attended, IMH endorsement, and RS/C provision; and
- Outcomes — social and emotional child outcomes measurement.
Analysis of these data can help state early intervention (Part C) programs examine the status of serving children with social and emotional delays, address any gaps, and evaluate change over time.
Recognizing that IECMH services may be provided to eligible children and families by other programs and organizations, state early intervention (Part C) programs may want to examine whether their data system can capture and report utilization regarding those services.
Considering the data that will be needed for an evaluation is an important step at the beginning of a new initiative or any new investment of funds and effort, and enables states to address issues regarding access to quality services.
Appendix A: State Spotlights
Alabama

In 2014, Alabama's system of Infant and Early Childhood Mental Health started with a federally funded Linking Actions for Unmet Needs in Children's Health (Project LAUNCH). The grant included hiring and training a cadre of IECMH consultants statewide, a reflective supervision lead, and staff. Alabama also funded an IECMH state coordinator position within the Department of Early Childhood Education to address policy development and systems building.
The IECMH state coordinator works closely with the Alabama Department of Mental Health—Infant and Early Childhood Mental Health Services director to build the IECMH system.
Alabama is piloting IECMH consultation with two EI provider agencies that includes:
- Tier 1: universal support, which is not child-specific and includes training for EI staff on the use of the Temperament and Atypical Behavior Scale (TABS);
- Tier 2: where EI practitioners bring cases to a team meeting for consultation; and
- Tier 3: where IECMH consultation is added under "psychological services" on the IFSP and includes consultation with the parent(s) and other team members.
The IECMH consultants can also facilitate referrals for dyadic treatment—with more than 35 clinicians trained in Child-Parent Psychotherapy (CPP) statewide.
A training module on social-emotional development and IECMH, was developed for early intervention practitioners that includes a focus on trauma-informed care, attachment, and other relevant topics. Alabama uses American Recovery Plan Act (ARPA) funds to support participation of contracted early intervention staff (therapists) who otherwise might not be able to attend the training. Alabama is also training clinicians in DC:0–5 to help them determine the need for dyadic therapy and to support the ability to bill Medicaid.
Colorado

In the mid-2000s, the Office of Behavioral Health piloted placing early childhood mental health consultants in community-based mental health centers in two Colorado counties.
This program was later moved to the newly formed Office of Early Childhood (OEC) where it expanded across the state and grew from 17 full time equivalent (FTE) positions to 34 FTE. Utilizing one-time stimulus funds, the Early Childhood Mental Health (ECMH) Consultation program was able to grow to 52 FTE. Consultation in Colorado is also funded by philanthropic and private partners, with grants from the Buell Foundation adding roughly 17 FTE to this program.
In 2020, House Bill 20-1053 codified the ECMH Consultation Program into law, requiring the OEC to establish a model of consultation with a competency and qualification structure, as well as a professional development plan for all consultants across the state.
The OEC is working with leaders in Health Care Policy & Financing (HCPF) to explore whether Medicaid funding is a sustainable and reasonable approach to supporting ECMH consultation services.
ECMH consultants are licensed mental health providers with early childhood and developmental backgrounds and are all trained in DC:0–5. These consultants often refer children to early intervention (Part C) for further evaluation and act as a resource for EI teams by providing information and guidance; however, they do not complete Part C evaluations, nor do they provide direct intervention services.
Early Intervention Colorado (Part C) requires that local EI agencies have social emotional providers on their teams when needed, who are from a variety of professional disciplines including: infant mental health specialists, behavior analysts, family therapists, counselors, social workers, psychologists, psychiatrists, and infant family specialists. Social emotional providers who conduct evaluations of social-emotional development are required to complete DC:0–5 training.
Connecticut

In 2013, the State of Connecticut passed Public Act 13-178: An Act Concerning the Mental, Emotional and Behavioral Health of Youths which required the Birth to Three Program (early intervention IDEA Part C) to "provide mental health services to any child eligible for early intervention services" as needed and "Any child not eligible for services under said act shall be referred by the program to a licensed mental health care provider for evaluation and treatment, as needed".
However, Birth To Three had already focused on supporting mental health of infants and toddlers in the context of their families. That included the publication of the Service Guideline 4: Infant Mental Health: Assessment and intervention guidance for service providers and families of young children (2009) that was developed collaboratively with the Connecticut Association for Infant Mental Health (CT-AIMH) and was a revision to a document developed in 1998.
The legislation put a focus on IECMH and led to changes regarding screening and evaluation. This also led to an increase in CAPTA referrals and establishing regular training to the child welfare agency staff regarding the referral process to Birth to Three.
The Connecticut Birth To Three System requires that a mental health clinician be on the evaluation team if the referral was made due to concerns regarding social-emotional development. Additionally, if the child does not meet eligibility based on use of a multi-domain tool, the mental health clinician administers the Devereaux Early Childhood Assessment: Infant and Toddler (DECA-I/T).
Georgia

In 2019, the Georgia House of Representatives formed a study committee, chaired by Representative Katie Dempsey, to examine Infant and Early Childhood Mental Health (IECMH). The study committee resulted in a report and a series of recommendations, including funding of an IECMH director position at the Georgia Department of Early Care and Learning (DECAL), a request for clarification on Medicaid billing codes for IECMH services, and investment in the IECMH workforce.
The work of the study committee also resulted in the Georgia Early Education Alliance for Ready Students (GEEARS) and the Georgia Department of Public Health (DPH) recognizing the need for additional social-emotional support for children in Georgia's Early Intervention program, Babies Can't Wait (BCW). DPH identified Child-Parent Psychotherapy (CPP) as a potential treatment that could benefit the children served in BCW.
GEEARS and DPH reached out to partners in Alabama and South Carolina to determine interest in jointly funded CPP training for clinicians across the three states. Alabama, having a history of investment in IECMH, offered slots in a CPP training event to clinicians in Georgia and South Carolina, thereby creating a regional CPP training cohort.
DECAL recognized that child care and Head Start would also benefit from CPP-trained clinicians and partnered with DPH and GEEARS to provide CPP training. DECAL and DPH planned to invest additional funds from the Preschool Development Grant Birth through Five (PDG B-5) and American Rescue Plan Act (ARPA) funds for the training of roughly 90 additional clinicians in Georgia.
Hawaii

Hawaii's Early Intervention Section (Part C) participated in a collaborative effort that was supported by the state Early Learning Board (the governing entity of the Executive Office on Early Learning) to develop a behavioral health action plan that would complement and augment existing plans, including the Early Childhood State Plan.
A cross-sector team and WestEd conducted a scan of the status of infant and early childhood mental health (IECMH) in Hawaii and conducted key informant interviews that resulted in Hawai'i's Integrated Infant and Early Childhood Behavioral Health Plan.
The plan proposes to integrate child and family mental health and trauma-informed care into health and early care and learning systems throughout Hawaii.
The plan includes goals and strategies to address the following components:
- systems and policy;
- marketing, outreach, and community education;
- workforce development and consultation; and
- programs and services.
Hawaii's collaborative IECMH effort has been financially and structurally supported by the Hawaii Community Foundation, the Early Childhood Action Strategy, and the State Department of Health. Foundations have also supported subsequent collaborative efforts to address funding for IECMH services and supports. Hawaii's Early Intervention Section (Part C) participated in this effort that resulted in the 2021 report Advancing Infant and Early Childhood Behavioral Health in Hawai'i: Exploring Options for Financing Sustainability, which examines sustainable funding for IECMH services, including information on diagnosis coding and billing, as well as potential funding sources.
A collaboration of philanthropic groups also supported an intensive nine-month-long trauma-informed Promising Minds Community of Practice (COP). The COP included a mixed group of early childhood professionals including early intervention, home visiting, child care, Early Head Start/Head Start, and family child interaction learning programs who reported that they gained knowledge and understanding of the impact of trauma on children, families and themselves and the importance of self-care, which proved to be very helpful during the COVID-19 pandemic.
Illinois

In 2016, Illinois created the Illinois Action Plan to Integrate Early Childhood Mental Health into Child- and Family-Serving Systems, Prenatal through Age Five to integrate IECMH into child-serving systems and has made strides expanding and evaluating Illinois Model of Infant/Early Childhood Mental Health Consultation (IECMHC) across the state.
The Illinois early intervention program has addressed the social and emotional development of infants and toddler for more than 20 years, with a committee established in 1999 and a report published in 2002 that identified social-emotional development as the primary unmet need of infants, toddlers, and families in early intervention.
The committee recommended having a social-emotional (SE) consultant within each of the 25 Child and Family Connections (CFC) offices (Illinois' system point of entry), training in relationship-based EI, reflective consultation for CFC leadership, reflective supervision for service coordinators, social-emotional screening at intake for all children, integrated assessment and intervention planning, regular case consultation, and a SE consultant network.
SE consultants must have a master's degree in child development, special education, psychology, social work, counseling or a related field, along with supervised clinical experience with children and families, and knowledge of and training in typical and atypical infant development, attachment theory, family systems theory, psychopathology in infancy and toddlerhood, diagnosis of mental health disorders in infancy (DC:0–5), impact of stress and trauma in infancy, assessment of parent/child relationship, intervention to support parent/child relationship, and assessment of adult mental health disorders.
Funded through a grant to each CFC, the SE consultants provide professional development, clinical consultation, and systems support for infusing relationship-based, reflective practice throughout the EI process. Primary responsibilities of the SE consultant also include reflective consultation to the CFC leadership, individual and group case consultation, and the coordination of SE screening and specialized assessment, with a social worker, counselor, or psychologist joining the assessment/evaluation team when screening results indicate a need.
Illinois' credentialing process for psychological and other counseling service providers, such as licensed psychologists, professional counselors, family therapists, and clinical social workers, can provide clinical dyadic therapy. Additionally, Illinois Early Intervention Training Program staff who participate in Training of Trainers to help build the capacity of early intervention/early childhood educators in the state.
Several SE consultants have also participated in training on DC:0–5. Recognizing the importance of support for young children with social-emotional challenges in early intervention, the Illinois Bureau of Early Intervention recently included diagnoses from DC:0–5 in the list of medical diagnoses that make children eligible for early intervention services.
Nevada

In 2019, The Nevada Early Intervention Services (Part C) program initiated statewide implementation of the Pyramid Model. Nevada was supported by NCPMI using implementation science and a systems approach to move from initial installation to implementation and scale-up.
A state leadership team uses the State Leadership Team Benchmarks of Quality for Implementing the Pyramid Model Statewide to put implementation and scale-up activities in place and track their progress. Program implementation coaches provide training and technical assistance to state-operated early intervention service agencies and community programs.
Training addresses Pyramid Model practices including program-wide leadership teaming, practice-based coaching, and use of data tools. Each local program forms a leadership team to guide implementation and plan for staff readiness and buy-in, family engagement, staff capacity, interventions for children with persistent challenging behavior, and the monitoring of implementation and outcomes (for example, using the Pyramid Model Early Intervention Benchmarks of Quality). The local leadership team decides how to provide ongoing practitioner coaching to help personnel develop proficiency to implement Pyramid Model practices. Practitioner coaches collaborate with early interventionists to identify strengths and areas for growth using the Early Interventionist Pyramid Practices Fidelity Instrument (EIPPFI) in collaboration. The leadership teams review data from the practitioner coach log and the EIPPFI to monitor implementation fidelity and make decisions related to ongoing professional development.
New York

In 2017, the New York State Department of Health Early Intervention Program published Meeting the Social-Emotional Development Needs of Infants and Toddlers: Guidance for Early Intervention Program Providers and Other Early childhood Professionals.
This document was the culmination of a joint taskforce convened in 2013 from two Governor-appointed bodies: The Early Intervention Coordinating Council (EICC), and the Early Childhood Advisory Council (ECAC).
The guidance document has four objectives:
- ensure that the general population of young children receive routine and ongoing screening of children's development, including social-emotional development;
- identify children at-risk of experiencing a social-emotional delay or disability and ensure that their families receive the assistance they need from the wide array of early childhood programs and services;
- improve the early identification of children who may already be experiencing developmental delays in social-emotional development; and
- ensure that evaluations and assessments for all children in the EI program adequately address social-emotional development, and that service coordinators, evaluators, and providers who are delivering EI services understand the importance of and pay attention to this area of development.
An EICC workgroup was created to help promote, disseminate, and train professionals on the guidance document. The workgroup created a social-emotional development webpage targeted towards families, as well as an online e-learning training for providers that includes five modules that provide specific instructions for early intervention professionals to address the social-emotional development of the children and families they serve.
New York State Department of Health Early Intervention Program is also part of a Trauma-Informed Collaborative that includes members from 15 state agencies, and is focused on promoting trauma-informed care and addressing social-emotional development.
North Carolina

There has been a broad interest across North Carolina agencies in promoting IECMH. This has included investments by the Division of Public Health making Triple P — Positive Parenting Program available across the state, as well as joint investments making available Circle of Security.
In 2017, as part of its State Systematic Improvement Plan (SSIP), the North Carolina Infant-Toddler Program (Part C) conducted a survey of early intervention providers regarding perceived IECMH strengths, resources and needs. Several implementation teams were established to address the results of the survey.
One action taken was to integrate IECMH competencies into the personnel standards for the Infant-Toddler (Part C) program. Two additional areas of focus and investment were to promote a family coaching approach with support from Dathan Rush and M'Lisa Shelden, which helped establish a foundation for working with families from a more dyadic perspective.
Additionally, North Carolina further promoted the Pyramid Model, which was already in use by other early childhood programs in the state, and the Infant-Toddler (Part C) program became a part of the state Pyramid Model leadership team.
North Carolina is also supporting the ABC: Attachment Biobehavioral Catchup, which is a rigorous mental health intervention, but implementation doesn't have to be by a mental health clinician. North Carolina also invested in the ASQ:SE-2, enabling provider agencies statewide to be able to use it and 50 clinicians have been trained in the DC:0–5 and will be training at least another 25.
The Infant-Toddler program has taken a leadership role in bringing the Association for the Advancement of IMH competencies and endorsement process to North Carolina, using Preschool Development Grant Birth through Five (PDG B-5) funds, and they are encouraging early intervention practitioners to become endorsed.
Michigan

The Michigan early intervention program, known as Early On, selected improving social emotional outcomes for infants, toddlers, and their families as the focus for their State Systemic Improvement Plan (SSIP). Initially, Early On Michigan selected four service areas as pilot sites to implement evidence-based practices and evaluate activities and is currently scaling up to implement them in one-third of the state. The evidence-based practices include:
- training and use of the electronic Devereaux Early Childhood Assessment for Infants and Toddlers (eDECA-I/T) that is sensitive enough to pick up social emotional concerns that other evaluation tools may miss; and
- Pyramid Model training (five modules) with coaching to support providers using the Pyramid Model.
Additionally, Early On Michigan decided to address messaging and improve awareness of the importance of social and emotional development. This included purchasing Social Emotional Developmental Wheels from Michigan Association for Infant Mental Health and ZERO TO THREE. Early intervention providers reported that this tool has made it easier to start having conversations with families about social-emotional development. A contract with the Michigan Department of Health & Human Services Mental Health (MDHHS) was also developed for a consultant to provide foundational training in areas such as temperament, attachment, typical and atypical development, nurturing environments, and social emotional milestones.
Early On Michigan determined that mental health providers can diagnose infant mental health conditions, that have been included in their list of physical and mental conditions that make a child eligible for early intervention (Part C). Additionally, Infant Mental Health Endorsement is promoted, encouraged, and included in the Early On Michigan's Personnel Standards.
Rhode Island

Since putting in place policies and procedures in 2005 to meet the Child Abuse Protection and Treatment Act (CAPTA) mandate for referral of children and their families when there is a substantiated case of abuse or neglect, Rhode Island has conducted a Continuous Quality Improvement (CQI) effort to address effective implementation of this requirement over several years.
A child welfare subcommittee (of the state Interagency Coordinating Council) conducted CQI that included reviewing data on referrals made, developmental screening conducted, and children determined eligible for early intervention (IDEA Part C). Policy changes that were made include developing: a CAPTA liaison position; a child welfare standardized referral protocol; standardized form and feedback loop so that child welfare knows the status of referral; as well training for both early intervention and child welfare staff.
Rhode Island also established a process where, unless there is an established delay or disability, referrals from child welfare are made to a home visiting entity First Connections (which receives some EI Part C funding) to conduct development screening (including ASQ:SE-2) and route referrals to home visiting when there is no risk of developmental delay identified. Rhode Island has a Family Visiting Council that works to align policies across home visiting programs and early intervention. The focus on CAPTA referrals has led to the need for the inclusion of social workers/mental health professionals on evaluation teams and recognition of the need for more professional development around IECMH.
Rhode Island's CAPTA work was featured in the following journal article:
- Bernstein, H., et al. (2020). Chance elevator encounters and tenacious champions: Collaborative referrals between child welfare and Early intervention, ZERO TO THREE Journal 40(6), 21–32.
Wisconsin

The Wisconsin Alliance for Infant Mental Health (WI-AIMH) in collaboration with the Wisconsin Child Welfare Professional Development System (WCWPDS) provides professional development across disciplines, including early intervention (Part C) practitioners, in training and coaching on the Facilitating Attuned Interactions (FAN) approach, as well as reflective supervision and IMH consultation.
Local Birth to 3 programs applied for competitive grants from the Wisconsin Birth to 3 Program (IDEA Part C) to pilot innovative practices that have a positive impact on the social and emotional development of the children they serve. Many awardees used some of their grant funds for professional development in social-emotional well-being, including training in the FAN Approach.
More than 100 providers attended the "Level 1" two-day interactive training and "Level 2" completion of reflection tools with supervisors who receive reflective coaching to support their teams for a period of six months.
Learners then participated in a third day of interactive training. After practitioners complete the training, they can participate in a Community of Practice (CoP) with others implementing the FAN Approach. These CoP sessions are offered one to two times per year to deepen knowledge and skills of practitioners in the field. The FAN Approach training is open to all early intervention disciplines and their supervisors. Mental health consultants are encouraged to attend with their team.
Training has also been provided in the Pyramid Model Parents Interacting With Infants and Toddlers (PIWI) module, as it is felt that the coaching process aligns with the approach of early intervention and provides additional skills and strategies for supporting the parent-child dyad with a focus on social emotional elements within that interaction.
WI-AIMH developed Reflective Supervision Learning Collaborative, an experiential opportunity for program supervisors to learn about, experience, and implement reflective supervision within their agencies. The training will occur over five days throughout the year, along with monthly small group reflective meetings facilitated by infant mental health consultants.
Additionally, as a part of supporting ongoing professional development, Wisconsin Birth to 3 Program provides annual scholarships for early intervention professionals to attend a year-long Infant, Early Childhood, and Family Mental Health Capstone Certificate Program at the University of Wisconsin. Nearly 100 fellows have gone through this Capstone Certification across the state.
Appendix B: State Early Intervention (Part C) and IECMH Planning Tool
State early intervention (Part C) programs and partners can use this tool to jointly examine the status of IECMH policies and practices, both statewide, and in local communities and regions. This can help identify gaps as well as exemplars that could be expanded or replicated.
The review can also identify activities that haven't yet been implemented in the state, and the prioritization of each activity. The tool can be used to explore possible next steps that may include some of the implementation strategies included in this paper. It is not expected that states will address all activities.
For each section, examine the listed elements using the following qualities:
- How high of a priority is this?
- What do we know about what's happening in our state?
- What are our possible next steps?
Suggested Priority Rating Scale
- 1 = High priority
- 2 = Medium priority
- 3 = Not a priority
- N/A = Not applicable
- CI = Currently implemented
1. Referral, Screening and Assessment, and Eligibility
- 1.1. Expand child find outreach efforts to the full range of providers and settings that serve children at-risk of social-emotional difficulties (for example, social service organizations, domestic violence/homeless shelters).
- 1.2. Encourage other early learning and care providers (for example, home visiting, child care, Early Head Start) and healthcare providers to screen for social and emotional development concerns.
- 1.3. Partner with the child welfare agency to examine CAPTA and CARA Plans of Safe Care policies and procedures to ensure timely and effective referrals of children with potential social-emotional delay and mental health issues dues to maltreatment and/or parental abuse use in utero.
- 1.4. Promote the use of screening tools that address social and emotional development.
- 1.5. Promote the use of a tool focused on social and emotional development as part of the evaluation to supplement the multi-domain tool used.
- 1.6. Promote the inclusion of a licensed mental health specialist or professional trained and/ or endorsed in IMH on the evaluation team when appropriate (for example, CAPTA referrals, when there are social and emotional development concerns or family risk factors), who may either be a member of the early intervention team or accessed through a partnership with another community organization.
- 1.7. Expand the list of diagnosed conditions for eligibility to include additional IECMH-related conditions including attachment disorder, posttraumatic stress, trauma, depressive and other mood disorders, eating, sleep, crying, and regulation disorders.
- 1.8. Partner with other organizations to provide training for mental health clinicians to help identify the presence of infant mental health conditions (for example, DC:0–5) that can also help teams determine whether the child and family could benefit from a referral for evidence-based IECMH intervention/treatment.
2. Services and Practices
- 2.1. Promote a focus on the importance of the social and emotional development and mental health of infants and toddlers within the context of relationships through a collaborative public awareness campaign.
- 2.2. Promote a basic understanding of IECMH and prevention and intervention practices that support healthy social and emotional development and parent-child relationships through professional development and guidance materials for early intervention practitioners, supervisors, and administrators.
- 2.3. Support implementation of preventive-intervention models/approaches (for example, reflective practice, FAN approach; Pyramid Model; NEAR@Home) utilizing "implementation science" strategies (for example, professional development, coaching, and supporting leadership).
- 2.4. Develop a system of IECMH consultation to support early intervention practitioners in identifying and better meeting the social-emotional needs of eligible infants and toddlers with mental health needs and supporting the parent-child relationship. This may be accomplished in collaboration with other early learning and care or mental health agencies or organizations.
- 2.5. Encourage relationships at the local level between early intervention (Part C) and local mental health professionals and organizations, such as community mental health agencies, local early childhood coalitions/groups, and associations of infant mental health to facilitate coordination of services.
- 2.6. Support access to evidence-based dyadic treatment when the parent-child relationship has been negatively affected by trauma or other family stressors. Clinicians trained in these approaches may be a part of early intervention teams or accessed through another program/organization.
- 2.7. Support access to evidence-based parenting programs that focus on positive parent-child relationships and parenting skills to promote the child's social-emotional growth.
- 2.8. Encourage early intervention teams to help adult family members access needed mental health, including supports (for example, screening/evaluation and treatment for mental health needs incl. post-partum depression, substance use disorder, and access to needed domestic violence support) that present challenges to the parent-child relationship.
3. Workforce Development
- 3.1. Incorporate IECMH topics into training modules for all early intervention practitioners, supervisors, and administrators, including ACEs, toxic stress, and the critical importance of early relationships for healthy social-emotional development and mental health of young children.
- 3.2. Make available training to EI practitioners on preventive-intervention models/approaches (for example, FAN approach; Pyramid Model; NEAR@Home) and reflective practice.
- 3.3. Make training available to mental health clinicians on evidence-based parenting groups and dyadic treatments.
- 3.4. Incorporate IMH competencies into the state early intervention competencies, where applicable.
- 3.5. Promote and encourage mental health professionals in early intervention to receive IECMH training and/or endorsement as Infant Mental Health Specialist (IMHS) category or Infant Mental Health Mentor-Clinical.
- 3.6. Promote and encourage some early intervention practitioners to become endorsed at the Infant Family Specialist (IFS) category.
- 3.7. Support the development of an infrastructure system of Reflective Supervision/Consultation (RS/C) to allow all early intervention personnel to receive regular and ongoing reflective supervision.
4. Funding, Partnership, and Collaboration
- 4.1. Examine state policy/standards/regulations, service definitions, codes, and rates to determine the ability to bill for IECMH services as part of the IFSP.
- 4.2. Meet with state Medicaid partners to examine Medicaid funding of IECMH services, including the use of applicable diagnosis codes.
- 4.3. Collaborate with the state mental health and/or IECMH leaders to explore how IECMH services can be made available to families eligible for early intervention (Part C).
- 4.4. Join or convene an IECMH collaborative workgroup with other agencies/organizations to explore braiding funding for IECMH services, professional development, and effective IECMH systems building.
- 4.5. Explore federal or philanthropic funding opportunities for IECMH systems building, professional development, etc.
References
- ACEs Aware (n.d.). ACE fundamentals: Adverse Childhood Experiences (ACEs) are not destiny. State of California Department of Health Care Services. https://www.acesaware.org/ace-fundamentals/
- American Academy of Pediatrics, & Bright Futures (2021). Recommendations for preventive pediatric health care. https://downloads.aap.org/AAP/PDF/periodicity_schedule.pdf
- Beck, C.T. (2015). Middle range theory of traumatic childbirth: the ever-widening ripple effect. Global Qualitative Nursing Research. January 2015. https://doi.org/10.1177/2333393615575313
- Bernstein, H.K., Hartman, L.A., Hebbeler, K., Kaufman, J.L., Magaw, D., Shaw, E.F., Schmidt, L.K., & Spiker, D. (2020). Chance elevator encounters and tenacious champions: collaborative referrals between child welfare and early intervention. ZERO TO THREE, 40(6), 21–32. https://www.zerotothree.org/resources/3538-chance-elevator-encounters-and-tenacious-champions-collaborative-referrals-between-child-welfare-and-early-intervention
- Bruder, M.B., Catalino, T., Chiarello, L.A., Mitchell, M.C., Deppe, J., Gundler, D., Kemp, P., LeMoine, S., Long, T., Muhlenhaupt, M., Prelock, P., Schefkind, S., Stayton, V., & Ziegler, D. (2019). Finding a common lens: competencies across professional disciplines providing early childhood intervention. Infants & Young Children, 32(4), 280–293. https://doi.org/10.1097/IYC.0000000000000153
- Burak, E.W., & Rolfes-Haase, K. (2018). Using Medicaid to ensure the healthy social and emotional development of infants and toddlers. Georgetown University, Health Policy Institute, Center for Children and Families. https://ccf.georgetown.edu/wp-content/uploads/2018/12/Medicaid-and-IECMH_FINAL.pdf
- Center for Early Education and Development (2019). Reflective supervision/consultation: preventing burnout, boosting effectiveness, and renewing purpose for frontline workers. University of Minnesota Center for Early Education and Development. http://www.traumainformedcareproject.org/resources/UMN-CEED-Reflective-Supervision-Consultation.pdf
- Center of Excellence for Infant & Early Childhood Mental Health Consultation (2020). Center of Excellence for Infant and Early Childhood Mental Health consultation competencies. https://www.iecmhc.org/documents/IECMHC-competencies.pdf
- Center on the Developing Child (2016). From best practices to breakthrough impacts: a science-based approach to building a more promising future for young children and families. Harvard University. https://eric.ed.gov/?id=ED594409
- Center on the Developing Child (n.d.). A guide to toxic stress. Harvard University. https://developingchild.harvard.edu/guide/a-guide-to-toxic-stress/
- Center on the Developing Child (2007). InBrief: the impact of early adversity on children's development. Harvard University. https://developingchild.harvard.edu/resources/inbrief-the-impact-of-early-adversity-on-childrens-development/
- Center on the Developing Child (2015). Resilience. Harvard University. https://developingchild.harvard.edu/science/key-concepts/resilience/
- Child Welfare Information Gateway. (2020). Plans of safe care for infants with prenatal substance exposure and their families. Washington, DC: U.S. Department of Health & Human Services, Administration for Children and Families, Children's Bureau. https://www.childwelfare.gov/resources/plans-safe-care-infants-prenatal-substance-exposure-and-their-families/
- Cosgrove, K., Gilkerson, L., Leviton, A., Mueller, M., Norris-Shortle, C., & Gouvêa, M. (2019). Building professional capacity to strengthen parent/professional relationships in early intervention: the FAN approach. Infants & Young Children, 32(4), 245–254. https://doi.org/10.1097/IYC.0000000000000148
- Division for Early Childhood of the Council for Exceptional Children (2022). Infant mental health CoP. https://www.dec-sped.org/infantmentalhealthcop
- Earls, M.F. (2010). Incorporating recognition and management of perinatal and postpartum depression into pediatric practice. Pediatrics, 126(5), 1032-1039. https://doi.org/10.1542/peds.2010-2348
- Early Childhood Personnel Center (n.d.). Cross-disciplinary competencies. University of Connecticut, Center for Excellence in Developmental Disabilities. https://ecpcta.org/cross-disciplinary-competencies/
- Early Childhood Technical Assistance Center (n.d.). Early intervention services: key principles and practices. FPG Child Development Institute, University of North Carolina. https://ectacenter.org/topics/eiservices/keyprinckeyprac.asp
- Early Childhood Technical Assistance Center (2015). A system framework for building high-quality early intervention and preschool special education programs. FPG Child Development Institute, University of North Carolina. https://ectacenter.org/sysframe/
- Eggbeer, L., Mann, T., & Seibel, N. (2007). Reflective supervision: past, present, and future. ZERO TO THREE, 28(2), 5–9.
- Fenichel, E. (1992). Learning through supervision and mentorship to support the development of infants, toddlers and their families: a source book. Distributed by ERIC Clearinghouse.
- FrameWorks Institute (2020). Building relationships: framing early relational health. Center for the Study of Social Policy. https://www.frameworksinstitute.org/resources/building-relationships-framing-early-relational-health/
- Goddard, J.A., Lehr, R., & Lapadat, J.C. (2000). Parents of Children with Disabilities: Telling a Different Story. Canadian Journal of Counselling and Psychotherapy, 34(4), 273–289. https://cjc-rcc.ucalgary.ca/article/view/58654
- Hambrick, E.P., Brawner, T.W., & Perry, B.D. (2019). Timing of early-life stress and the development of brain-related capacities. Frontiers in Behavioral Neuroscience, 13. https://doi.org/10.3389/fnbeh.2019.00183
- Harris, N.B. (2019). Written statement before the United States House of Representatives Education and Labor Committee. https://www.congress.gov/116/meeting/house/109904/witnesses/HHRG-116-ED14-Wstate-BurkeHarrisN-20190911.pdf
- Hayes S.A., & Watson, S.L. (2013). The impact of parenting stress: a meta-analysis of studies comparing the experience of parenting stress in parents of children with and without autism spectrum disorder. Journal of Autism and Developmental Disorders, 43(3), 629–42. https://doi.org/10.1007/s10803-012-1604-y
- Heller, S.S., & Gilkerson, L. (2009). A practical guide to reflective supervision. ZERO TO THREE.
- IDEA Infant & Toddler Coordinators Association (2019). IDEA Infant Toddler Coordinators Association early intervention birth cohort study: an alternative Approach to measuring child & family participation in Part C of IDEA. https://www.ideainfanttoddler.org/pdf/ITCA-Birth-Cohort-Report-2019.pdf
- IDEA Infant & Toddler Coordinators Association (2018). 2018 finance survey report. https://www.ideainfanttoddler.org/pdf/Finance-Survey-Report-Pt-1-Executive-Summary-Fund-Utilization.pdf
- Innocenti, M.S., Roggman, L.A., & Cook, G.A. (2013). Using the PICCOLO with parents of children with a disability. Infant Mental Health Journal, 34(4), 307–318. https://doi/10.1002/imhj.21394
- Johnson-Motoyama, M., Moses, M., Conrad-Hiebner, A., & Mariscal, E. S. (2016). Development, CAPTA Part C referral and services among young children in the U.S. child welfare system. Child Maltreatment, 21(3), 186–197. https://doi.org/10.1177/1077559516630831
- Kaiser Commission on Medicaid and the Uninsured (2012). Medicaid financing: An overview of the federal Medicaid matching rate (FMAP). Kaiser Family Foundation. https://www.kff.org/wp-content/uploads/2013/01/8352.pdf
- Kaiser Family Foundation (n.d.). Federal medical assistance percentage (FMAP) for Medicaid and multiplier. https://www.kff.org/medicaid/state-indicator/federal-matching-rate-and-multiplier
- Lancaster, C.A., Gold, K.J., Flynn, H.A., Yoo, H., Marcus, S.M., & Davis, M.M. (2010). Risk factors for depressive symptoms during pregnancy: a systematic review. American Journal of Obstetrics and Gynecology, 202(1), 5–14. https://doi.org/10.1016/j.ajog.2009.09.007
- Mann, C., Serafi, K., Eder, J., & O'Connor, K. (2019). Keeping Medicaid's promise for children with special health needs. Manatt. https://www.manatt.com/insights/newsletters/manatt-on-health-medicaid-edition/keeping-medicaids-promise-for-children
- Medicaid and CHIP Payment and Access Commission (2019). CHIP health services initiatives: what they are and how states use them. https://www.macpac.gov/wp-content/uploads/2019/07/CHIP-Health-Services-Initiatives.pdf
- Michigan Association for Infant Mental Health (2017). Competency guidelines: endorsement for culturally sensitive, relationship-focused practice promoting infant mental health. https://www.infancyonward.org/wp-content/uploads/2021/03/IMH-ECMH-Competency-Guidelines.pdf
- Morris, C.T., Hunter, A., Fox, L., & Hemmeter M.L. (2021). The Pyramid Model and trauma-informed care: a guide for early childhood professionals to support young children's resilience. National Center for Pyramid Model Innovations. https://challengingbehavior.cbcs.usf.edu/docs/Trauma-Informed-Care_Guide.pdf
- National Scientific Council on the Developing Child. (2019). Young children develop in an environment of relationships. Center on the Developing Child, Harvard University. https://developingchild.harvard.edu/resources/working-paper/wp1/
- New York State Association for Infant Mental Health (n.d.). What is reflective practice?. New York State Association for Infant Mental Health. https://www.nysaimh.org/reflective-practice/
- New York State Department of Health Early Intervention Program. (2017). Meeting the social-emotional development of infant and toddlers: guidance for early intervention program providers and other early childhood professionals. New York State Department of Health Early Intervention Coordinating Council, New York State Council on Children and Families Early Childhood Advisory Council, Joint Task Force on Social-Emotional Development. https://www.health.ny.gov/publications/4226.pdf
- Perry, B.D., & Szalavitz, M. (2017). The boy who was raised as a dog and other stories from a child psychiatrist's notebook: what traumatized children can teach us about loss, love, and healing. Basic Books.
- Phillips, D., & Shonkoff, J.P. (2000). From neurons to neighborhoods: the science of early childhood development. National Academies Press.
- Schecter, R., Pham, T., Hua, A., Spinazzola, R., Sonnenklar, J., Li, D., Papaioannou, H., & Milanaik, R. (2019). Prevalence and longevity of PTSD symptoms among parents of NICU infants analyzed across gestational age categories. Clinical Pediatrics, 59(2), 163–169. https://doi.org/10.1177/0009922819892046
- Smith, B.J., Fox, L., Strain, P., Binder, D.P., Bovey, T., Jones, A., McCullough, K., Veguilla, M., Dunlap, G., Blase, K., Trivette, C.M., Shapland, D., and Danaher, J. (2018). Statewide Implementation Guide. Early Childhood Technical Assistance Center, FPG Child Development Institute, University of North Carolina. https://ectacenter.org/sig
- Smith, S., Ferguson, D., Burak, E.W., Granja, M.R., & Ortuzar, C. (2020). Supporting social-emotional and mental health needs of young children through Part C early intervention: results of a 50-state survey. National Center for Children in Poverty. https://www.nccp.org/publication/part-c-report/
- Smith, S., Granja, M.R., Nguyen, U.S., & Rajani, K. (2018). How states use Medicaid to cover key infant and early childhood mental health services: results of a 50-state survey (2018 update). National Center for Children in Poverty. https://www.nccp.org/wp-content/uploads/2018/11/text_1211.pdf
- Stahmer, A.C., Leslie, L.K., Hurlburt, M., Barth, R.P., Webb, M.B., Landsverk, J., & Zhang, J. (2005). Developmental and behavioral needs and service use for young children in child welfare. Pediatrics, 116(4), 891–900. https://doi.org/10.1542/peds.2004-2135
- Substance Abuse and Mental Health Services Administration's Trauma and Justice Strategic Initiative (2014). SAMHSA's concept of trauma and guidance for a trauma-informed approach. U.S. Department of Health & Human Services, Substance Abuse and Mental Health Services Administration Office of Policy, Planning and Innovation. https://www.health.ny.gov/health_care/medicaid/program/medicaid_health_homes/docs/samhsa_trauma_concept_paper.pdf
- U.S. Department of Education, Office of Special Education and Rehabilitative Services (2021). Supporting child and student social, emotional, behavioral, and mental health needs. https://www2.ed.gov/documents/students/supporting-child-student-social-emotional-behavioral-mental-health.pdf
- U.S. Department of Health & Human Services, Administration for Children and Families, Administration on Children, Youth and Families, Children's Bureau (2021). Child maltreatment 2019. https://www.acf.hhs.gov/sites/default/files/documents/cb/cm2019.pdf
- Walsh, T.B., Davis, R.N., & Garfield, C. (2020). A call to action: screening fathers for perinatal depression. Pediatrics, 145(1). https://publications.aap.org/pediatrics/article-abstract/145/1/e20191193/36978/A-Call-to-Action-Screening-Fathers-for-Perinatal
- Weatherston, D.J., & Shirilla, J.J. (Eds.) (2002). Case studies in infant mental health: risk, resiliency, and relationships. ZERO TO THREE.
- Weatherston, D.J, & Eidson, F. (2019). Reflective supervision: co-construction of a relationship. Presented at the 2019 MI-AIMH Biennial Conference. https://mi-aimh.org/wp-content/uploads/2019/04/E1-Weatherston-5.pdf
- Williams, M.E., Zamora, I., Akinsilo, O., Chen, A.H., & Poulsen, M.K. (2017). Broad developmental screening misses young children with social-emotional needs. Clinical Pediatrics, 57(7), 844–849. https://doi.org/10.1177/0009922817733700
- Zeanah, C.H., Carter, A.S., Cohen, J., Egger, H., Gleason, M.M., Keren, M., Lieberman, A., Mulrooney, K., & Oser, C. (2017). Introducing a new classification of early childhood disorders: DC:0–5. ZERO TO THREE. https://mi-aimh.org/wp-content/uploads/2017/11/2017-01-Zeanah-S.-intro-article.pdf
- Zeanah, C.H. (2019). Handbook of infant mental health, fourth edition. The Guilford Press.
- ZERO TO THREE (2017). Infant and early childhood mental health consultation: a briefing paper. https://www.zerotothree.org/resources/1952-infant-and-early-childhood-mental-health-consultation-a-briefing-paper
- ZERO TO THREE (2016). Three building blocks of reflective supervision. https://www.zerotothree.org/resources/412-three-building-blocks-of-reflective-supervision
- ZERO TO THREE, & Manatt (2016). Planting seeds in fertile ground: steps every policymaker should take to advance infant and early childhood mental health. https://www.zerotothree.org/resources/1221-planting-seeds-in-fertile-ground-steps-every-policymaker-should-take-to-advance-infant-and-early-childhood-mental-health











